Drowning is the process of experiencing respiratory impairment from submersion/immersion in liquid. In a drowning event the person involved usually dies within 24 hours after submersion in water, however if the person involved in the event survives, it is called near drowning.
Near drowning(or submersion injury) is the survival of a drowning event involving unconsciousness or water inhalation and can lead to serious secondary complications, including death, after the event, caused by oxygen starvation secondary to the drowning in water. It is often caused through aspiration of water into the lungs while attempting to breathe.
Near drowning may also be a results of a person having spasms or muscle contractions, including loss of airway reflexes. This leads through the uncontrolled and uninhibited entry of water through the persons windpipe(Trachea) and therefore to Aspiration. Aspiration leads to oxygen not passing through the windpipe(Trachea) to the lungs and therefore the person suffocates with hypoxia(lack of oxygen). This leads to a loss in consciousness and often in Cardiac Arrest.
The person surviving a near drowning event and aspirating fluids into the lungs is at high risk of developing an inflammation in the lungs that can easily develop into lung failure or Adult Respiratory Distress Syndrome (ARDS).
The person drowning is also at high risk of hypothermia(cold temperature)
According to the World Health Organization(WHO), drowning is the 3rd leading cause of unintentional injury death worldwide, accounting for 7% of all injury related deaths (est. 388,000 deaths by drowning in 2004, excluding those due to natural disasters), with 96% of these deaths occurring in low- and middle-income countries.In many countries, drowning is one of the leading causes of death for children under 12 years old. For example, in the United States, it is the second leading cause of death (after motor vehicle crashes) in children 12 and younger. The rate of drowning in populations around the world varies widely according to their access to water, the climate and the national swimming culture.
Drowning itself is quick and silent, although it may be preceded by distress which is more visible. A person drowning is unable to shout or call for help, or seek attention, as they cannot obtain enough air. The instinctive drowning response is the final set of autonomic reaction in the 20 – 60 seconds before sinking underwater, and to the untrained eye can look similar to calm safe behavior. Lifeguards and other persons trained in rescue learn to recognize drowning people by watching for these instinctive movements.
- What are the causes of Near Drowning?
- What happens in Intensive Care?
- How long will your loved one remain in ICU?
- References
What are the causes of near drowning?
Approximately 90% of drownings take place in freshwater (rivers, lakes and swimming pools) and 10% in seawater. Drownings in other fluids is rare, and often relates to industrial accidents.
- Rip currents
- Accidental fall into water
- Head and Spinal injury
- Loss of consciousness
- Heart attacks or abnormal heart rhythms
- Drug and alcohol influence
- Road traffic accident near water
- Child abuse
- Suicide
- Murder
A continued lack of oxygen in the brain, hypoxia, will quickly render a person unconscious. An unconscious victim rescued with an airway still sealed from laryngospasm stands a good chance of a full recovery. Artificial respiration is also much more effective without water in the lungs. At this point the victim stands a good chance of recovery if attended to within minutes. Latent hypoxia is a special condition leading to unconsciousness where the partial pressure of oxygen in the lungs under pressure at the bottom of a deep free-dive is adequate to support consciousness but drops below the blackout threshold as the water pressure decreases on the ascent, usually close to the surface as the pressure approaches normal atmospheric pressure. A blackout on ascent like this is called a deep water blackout.
The brain cannot survive long without oxygen and the continued lack of oxygen in the blood combined with the cardiac arrest will lead to the deterioration of brain cells causing first brain damage and eventually Brain Death from which recovery is generally considered impossible.
A lack of oxygen or chemical changes in the lungs may cause the heart to stop beating; this Cardiac Arrest stops the flow of blood and thus stops the transport of oxygen to the brain. Cardiac arrest used to be the traditional point of death but at this point there is still a chance of recovery. The brain will die after approximately six minutes without oxygen but special conditions may prolong this.

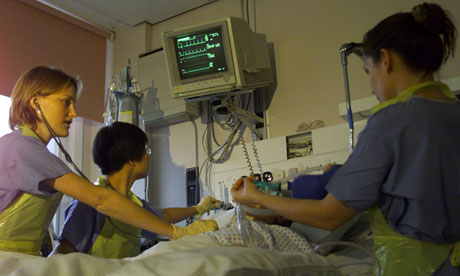
What happens in Intensive Care?
- Your loved one is continuously monitored with a Bedside Monitors– Your loved ones vital signs such as Blood pressure is usually displayed continuously on the bedside monitor via an Arterial Catheter. Your loved ones Heart, Heart rhythm(ECG), temperature and breathing rate is continuously monitored and displayed on the monitor. Oxygen levels are continuously monitored by an oxygen saturation probe attached to the finger or to the ear. Furthermore oxygen levels are intermittently checked with ABG’s(Arterial Blood Gases), where blood is drawn out of the Arterial Catheter and tested immediately via a Blood Gas Analyser.
- Your loved ones breathing will be supported by additional oxygen via an oxygen mask, or Non- Invasive Ventilation(NIV) or BIPAP ventilation, however it is most likely that your loved requires full ventilation on a Ventilator (Breathing Machine) and have a Breathing Tube (Endotracheal tube) inserted into their airway. Most Patients suffering from near drowning events are in an induced Coma and therefore require mechanical ventilation with a Ventilator (Breathing Machine).
- If your loved one has a head or brain injury he or she may require Intracranial Pressure Monitoring, which basically monitors the pressure in your loved ones head
- Your loved one will be receiving intravenous fluids via several intravenous cannula’s or Central Venous Lines(central line or CVC). A Urinary Catheter is used to monitor urine output and a Nasogastric Tubes will be used to rest the intestine if this has been injured or if your loved one requires ventilation
- You can expect your loved one to have frequent Chest X-rays and blood tests(Blood& Pathology tests in Intensive Care) especially arterial blood gases (ABGs)
- Your loved one will be receiving intravenous fluids via several intravenous cannula’s or Central Venous Lines(central line or CVC). A Urinary Catheter is used to monitor urine output and a Nasogastric Tubes will be used to rest the intestine if this has been injured or if your loved one requires ventilation
- A warming blanket may be applied to correct hypothermia, as near drowning Patients are often very cold due to being submerged in water of low temperature
- Your loved one may have other associated injuries (spinal injury, bone fractures etc), which will also be managed in the intensive care unit.
While in the Intensive Care Unit, your loved one may have tests including chest x-rays and CT scans. Assessment of neurological status (brain activity), including any seizure activity is an important aspect in looking after the near drowning Patient, as a lack of oxygen to the brain may result in seizures.
How long will your loved one remain in Intensive Care?
The length of stay in Intensive Care, as well as the prognosis depends on how long your loved one was submerged in water and if there were any other associated injuries. Please ask the ICU nurse or doctor, as the time your loved one remains in ICU varies from person to person.
Reference
http://www.usla.org/ USA life saving association
The Royal Life Saving Society Australia
Any Questions?
Of course, if you have any questions or concerns, please discuss them with the ICU nurses and doctors.
All Intensive Care interventions and procedures carry a degree of potential risk even when performed by skilled and experienced staff. Please discuss these issues with the medical and nursing staff who are caring for your loved one.
The information contained on this page is general in nature and therefore cannot reflect individual Patient variation. It is meant as a back up to specific information which will be discussed with you by the Doctors and Nurses caring for your loved one. INTENSIVE CARE HOTLINE attests to the accuracy of the information contained here BUT takes no responsibility for how it may apply to an individual Patient. Please refer to the full disclaimer.
How can you have PEACE OF MIND, control, power and influence whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below! In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care! Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 “killer” tips& strategies helping you to get on the right path to PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care(it’s not what you think)