What is a Cardiac arrest?
Cardiac arrest, also known as cardiopulmonary arrest or circulatory arrest, is the cessation of normal circulation of the blood due to failure of the heart to contract effectively. Medical personnel may refer to an unexpected cardiac arrest as a sudden cardiac arrest (SCA).
A cardiac arrest is different from (but may be caused by) a Heart Attack(Acute Myocardial Infarction) where blood flow to the muscle of the heart is impaired.
Arrested blood circulation prevents delivery of oxygen to the body. Lack of oxygen to the brain causes loss of consciousness, which then results in abnormal or absent breathing. Brain injury is likely if cardiac arrest goes untreated for more than five minutes. For the best chance of survival and neurological recovery, immediate and decisive treatment is imperative.
Cardiac arrest is a medical emergency that, in certain situations, is potentially reversible if treated early. Unexpected cardiac arrest sometimes leads to death almost immediately; this is called sudden cardiac death (SCD).The treatment for cardiac arrest is cardiopulmonary resuscitation (CPR) to provide circulatory support, followed by defibrillation if a shockable rhythm(VT or VF) is present.
- What does the cardiovascular system do?
- Poor or abnormal function of the cardiovascular system
- Cardiac Arrest-(Heart Attack) Pathophysiology
- General Treatment Options
- What Happens in Intensive Care?
- How long will your loved one remain in Intensive Care?
What does the cardiovascular system do?
The essential components of the human cardiovascular system are the heart, lungs, blood, and blood vessels. It includes: the pulmonary circulation, a “loop” through the lungs where blood is oxygenated and the systemic circulation, a “loop” through the rest of the body to provide oxygenated blood. An average adult contains five to six quarts (roughly 4.7 to 5.7 liters) of blood, accounting for approximately 7% of their total body weight. Blood consists of plasma, red blood cells, white blood cells, and platelets. Also, the digestive system works with the circulatory system to provide the nutrients the system needs to keep the heart pumping.
The heart is at the centre, basically distributing blood from the ‘central pump’ with the blood vessels the pipes of the body, trying to reach every corner of the body. The cardiovascular system also passes nutrients (such as amino acids, electrolytes and lymph), gases(Oxygen and Carbon Dioxide), hormones, blood cells, etc. to and from cells in the body to help fight diseases, stabilize body temperature and pH, and to maintain blood pressure.
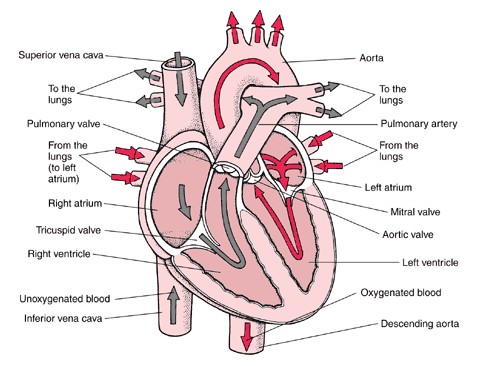
In the heart there is one atrium and one ventricle for each circulation, and with both a systemic and a pulmonary circulation there are four chambers in total: left atrium, left ventricle, right atrium and right ventricle. The right atrium is the upper chamber of the right side of the heart. The blood that is returned to the right atrium is de-oxygenated (poor in oxygen) and passed into the right ventricle to be pumped through the pulmonary artery to the lungs for re-oxygenation(inhalation) and removal of carbon dioxide(exhalation). The left atrium receives newly oxygenated blood from the lungs as well as the pulmonary vein which is passed into the strong left ventricle to be pumped through the aorta to the different organs of the body.The left side of the heart then receives oxygen rich blood from the lungs and pumps this blood into the Aorta and arteries of the body. This pumping action is a complex well-coordinated activity that cannot be fully explained here. The heart itself, receives oxygenated blood supply via the left and right coronary arteries.
Poor or abnormal function of the cardiovascular system
May be a result of:
- Insufficient blood supply due to dehydration, bleeding or swelling;
- Insufficient blood supply to the heart due to ‘clotted’ arteries
- A poor blood supply to the heart, where there is not enough oxygen and other nutrients for its work;
- Poor lung function or obstruction to blood flow in the lungs, which places a strain on the heart muscle;
- Too many or too few electrolytes (eg. potassium, magnesium) that cause irregular heartbeats or dangerous rhythms in the heart.
- Weakness of blood vessel walls
- Heart muscle weakness Cardiomyopathy
- unhealthy lifestyle such as alcohol consumption, smoking, obesity
Cardiac Arrest-(Heart Attack) Pathophysiology
Cardiac arrest, also known as cardiopulmonary arrest or circulatory arrest, is the cessation of normal circulation of the blood due to failure of the heart to contract effectively. A cardiac arrest is different from (but may be caused by) a Heart Attack(Acute Myocardial Infarction) where blood flow to the muscle of the heart is impaired.
Other conditions leading to Cardiac Arrest include a large brain hemorrhage, severe chest trauma, severe multi trauma with a large blood loss and massive chest contusion, imbalances of body chemicals such as Magnesium or Potassium or heart rhythm irregularities.
When a person has a cardiac arrest they usually collapse, become unconscious, they stop breathing and they loose their pulse. If this is the case, it is of vital necessity to commence CPR(Cardiopulmonary Resuscitation) ASAP, as three minutes or more without oxygen can cause irreversible brain damage. Other organs suffer from lack of oxygen as well. It is also necessary to call an ambulance if you witness a cardiac arrest.
The prognosis of a person having a cardiac arrest is dependent on a number of things, including how quickly and how effectively CPR was commenced and how long it takes for the heart to beat again, in what rhythm it beats and whether its beating is effective. It also depends on the persons pre-medical history. The time from when a person’s heart stops to the time it starts beating again is also known as ‘down-time’.
General Treatment Options
If a person is suffering a cardiac arrest it is of utmost importance to commence CPR(Cardiopulmonary Resuscitation) as quickly as possible. An Ambulance needs to be called as well as quickly as possible. CPR should be continued until emergency services/Ambulance arrives so that they can continue CPR, whilst also monitoring the Patient’s heart and decide treatment options depending on the hearts rhythm. Treatment may include defibrillation with defibrillation pads on a Person’s chest. If the Person survives the Cardiac Arrest at the scene, a transfer to a hospital into the Emergency Department and then to Intensive Care or Coronary Care for further management are the next steps. Ongoing treatment may include Angiogram and Cardiac Stenting(Angioplasty), Thrombolysis, Open Heart surgery(Coronary Artery Bypass Graft (CABG) surgery), Intra-Aortic Balloon Pump (IABP) therapy, ECMO(Extracorporeal Membrane Oxygenation) Therapy, but will be dependent on the causes of the cardiac arrest.
What Happens in Intensive Care?
Treatment for your loved one who has suffered a cardiac arrest may be straightforward or quite complex depending on the individual Patient and their immediate condition post cardiac arrest. Investigations such as blood tests, chest x-rays, CT, ultrasound of the heart etc… are performed to identify the cause of the cardiac arrest and treatment will be commenced accordingly. Further investigations will be required if your loved one does not regain consciousness in a short time.
- Initially oxygen and respiratory support might be commenced via na oxygen mask or via Non- Invasive Ventilation(NIV) or BIPAP ventilation
- Full ventilation using a Ventilators(Breathing Machine) and a Breathing Tube (endotracheal tube) will usually be required to improve and maintain the oxygen delivery
- Sedation may be used if your loved one is in an induced coma
- Your loved one will require monitoring using a Bedside Monitors and an Arterial Catheter(Arterial Line)
- You can expect your loved one to have frequent Chest X-rays and blood tests(Blood& Pathology tests in Intensive Care) especially arterial blood gases (ABGs)
- Infusion pumps are administering drugs to support your loved ones blood pressure and haemodynamic system, as well as intravenous fluids may be administered via a central venous catheter/ CVC(Central Venous Lines)
- Use of a Pulmonary Artery Catheters or a PICCO catheter to closely monitor cardiac function is not uncommon.
- An NG Tube (Nasogastric Tubes) is usually inserted into your loved ones stomach, in order to commence nutrition or to remove fluids
- Urine Output is usually measured hourly, after insertion of a Urinary Catheter
- If your loved one has suffered a severe cardiac arrest and is unconscious he or she may be ‘cooled'(therapeutic hypothermia after cardiac arrest) with a cooling blanket, for up to 24 hours to protect the brain and other organs.
How long will your loved one remain in Intensive Care?
The prognosis for out-of-hospital cardiac arrest are generally not good, with many people not surviving the cardiac arrest before even getting to the hospital. Patients who require CPR for more than three minutes are in danger of suffering a hypoxic brain injury, as their brain didn’t get enough oxygen during the cardiac arrest. If your loved one requires Intensive Care, the Doctors and Nurses explain the situation, treatment options(if any) and the prognosis of your loved one. Generally speaking the longer the cardiac arrest and the longer CPR has been performed and the longer your loved one remains in a coma the poorer the outlook and prognosis.
Any Questions?
Of course, if you have any questions or concerns, please discuss them with the ICU nurses and doctors.
All Intensive Care interventions and procedures carry a degree of potential risk even when performed by skilled and experienced staff. Please discuss these issues with the medical and nursing staff who are caring for your loved one.
The information contained on this page is general in nature and therefore cannot reflect individual Patient variation. It is meant as a back up to specific information which will be discussed with you by the Doctors and Nurses caring for your loved one. INTENSIVE CARE HOTLINE attests to the accuracy of the information contained here BUT takes no responsibility for how it may apply to an individual Patient. Please refer to the full disclaimer.
Related articles:
- How long does a cardiac arrest patient stay in Intensive Care?
- Six weeks in Intensive Care after Cardiac Surgery and my mother isn’t getting any better…
- How long can a breathing tube or an endotracheal tube can stay in?
- How long should a Patient be on a ventilator before having a Tracheostomy?
- How long is a Patient kept on a BIPAP machine in Intensive Care?
- What is an induced coma and why is my critically ill loved one in an induced coma?
- The 3 most dangerous mistakes that you are making but you are unaware of, if your loved one is a critically ill Patient in Intensive Care
- How to always achieve your goals whilst your loved one is critically ill in Intensive Care
- Why you must make up your own mind about your critically ill loved one’s situation in Intensive Care even if you’re not a doctor or a nurse!
- Follow this proven 5 step process on how to be in control and influential if your loved one is a long-term Patient in Intensive Care
- How to quickly take control and have real power and influence if your loved one is critically ill in Intensive Care
- Why does my loved one need a Tracheostomy in Intensive Care?
- Tracheostomy and weaning off the ventilator in Intensive Care, how long can it take?
- My sister has been in ICU for 21 weeks with Tracheostomy and still ventilated. What do we need to do?
- Severe lung failure and my aunty is not expected to survive…
- Be more selfish if your loved one is critically ill in Intensive Care
- How to stay positive if your loved one is critically ill in Intensive Care
- 4 ways on how to be more persuasive if your loved one is critically ill in Intensive Care
- 3 quick steps on how to position and prepare yourself well mentally, whilst your loved one is critically ill in Intensive Care
- How to get what you want whilst your loved one is critically ill in Intensive Care
- 5 steps to become a better negotiator if your loved one is critically ill in Intensive Care
- 5 Ways to have control, power and influence while your loved one is critically ill in Intensive Care
- How to make sure that your values and beliefs are known whilst your loved one is critically ill in Intensive Care
- How to make sure that “what you see is always what you get” whilst your loved one is critically ill in Intensive Care
- What the doctors and the nurses behaviour in Intensive Care is telling you about the culture in a unit
- How long does it take to wake up from a Traumatic brain injury or severe head injury
- How to take control if your loved one has a severe brain injury and is critically ill in Intensive Care
- Family Meetings in Intensive Care or the Elephant in the Room
- What you need to do if your loved one is dying in Intensive Care(part one)
- What you need to do if your loved one is dying in Intensive Care(part two)
- Intensive Care at its best?
- How INTENSIVECAREHOTLINE.COM Can Help You
- What you and your Family need to do if your critically ill loved one is very sick in Intensive Care and faces an uncertain future
- How long can somebody stay in Intensive Care?
- My Family can’t agree on what’s best for my sister in Intensive Care…Help!
- My husband is dying in Intensive Care, but we need more time…
- My mother sustained serious brain damage after a stroke and she now is in multi- organ failure


