What is Temporary Cardiac Pacing?
Temporary Cardiac Pacing is the temporary delivery of electrical impulses, delivered by electrodes contacting the heart muscles, to regulate and automate the beating of the heart. The primary purpose of temporary cardiac pacing is to maintain an adequate heart rate, either because the heart’s native(intrinsic) pacemaker is not fast enough, or there is a block in the heart’s electrical conduction system.
In Intensive Care Temporary Cardiac Pacing is instigated by a pacing box that is attached to small electrodes(pacing wires) that are connected to the Patient’s heart muscle. Those small electrodes(pacing wires) are usually implanted during cardiac surgery(Coronary Artery Bypass Graft (CABG) or they have been inserted through a vein, either a Central Line(Central Venous Lines) or a Swan-Ganz Cather(Pulmonary Artery Catheters). In either case pacing has been instigated as a temporary measure and once your loved one is stable and the heart is back in their own normal rhythm, pacing is superseded. In some cases temporary pacing may lead to permanent pacing and if the case it would lead to a pacemaker or defibrillator implant.
- How does a normal heartbeat occur?
- What can go wrong with the Heart Rhythm?
- Why is it done?
- What are the Risks?
- Publication
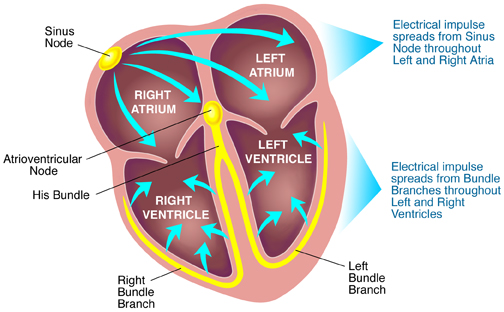
How does a normal heartbeat occur?
Normally the adult heart beats 60-100 beats per minute. This is also known as the pulse rate. This normal heart rate in a healthy person, ensures adequate blood pressure through adequate contracting of the heart muscle. This is an essential function to deliver enough oxygen and nutrients to the body’s organs and tissues.
The heart has an intrinsic/internal electrical conduction system that is a transmitter of electrical activity(current) that is transmitted from the Atrial Node all the way through the heart down to the Atrioventricular node. The intrinsic/internal electrical conduction system is made up of specialised tissue called nodes and fibres. Each heartbeat follows the electrical current from the Atrial Node all the way through the heart down to the Atrioventricular node(top to bottom). The electrical current or electrical impulse causes the heart muscle to contract and pushes blood from the atrium to the ventricle and also pushes blood from the ventricles into the body.
What can go wrong with the Heart Rhythm?
As explained above, if the conduction system fails to work in order(top to bottom) this can lead to different types of irregular heart rhythms(arrhythmia’s).
The most common types of arrhythmias that may lead to pacing are
- Atrial Fibrillation(AF)
- Atrial Flutter
- Junctional rhythm
- Heart blocks
- Sinus Bradycardia
- Ventricular Tachycardia(VT)
- Ventricular Fibrillation(VF)
If the conduction system fails to work in order, it means that the electrical current can fire from anywhere in the conduction system, leading to an uncoordinated and therefore irregular heartbeat. This can lead to low blood pressure and hypoxia(lack of oxygen) as less blood reaches the tissues, organs and cells.
A failed and uncoordinated conduction system can also lead to the atrium and the ventricle beating non- synchronous or independently. That can lead to differences in the heart rate in the atrium and the ventricle, leading to a heart block.


A battery powered pacing box (see figure above) is attached by cables to the pacing wires. An electrical pathway is set up between the pacing box and the heart.
Why is it done?
Temporary cardiac pacing is used to maintain a normal heart rate in Patients whose own heart rate is not pumping enough blood around the body. This may be in slow heart rhythms (bradycardia or heart blocks), fast rhythms (atrial fibrillation or ventricular tachycardia or when the heart fails to beat (sick sinus syndrome). Temporary cardiac pacing may be used when:
- Following a heart attack (acute myocardial infarction);
- Following cardiac surgery;
- Awaiting insertion of a permanent pacemaker;
- When the heart stops beating(cardiac arrest).
- It can also be used to make the heartbeat faster in order to over ride an undesirable rhythm.
What are the risks?
In Patients where temporary cardiac pacing has been established by placing a catheter into the heart via a large blood vessel or after surgery, complications may include:
- Bleeding at the insertion site
- malfunction of the pacemaker through empty batteries(normally the pacemaker and the batteries need to be checked 2-3 times a day)
- Infection (more likely if the wire is left in place for several days), normally the wire should be removed within 3-4 days after insertion
- Internal bleeding at the entry site of the wire to the heart(very rare)
- Pneumothorax through puncturing of the lung(rare)
- Hiccup, if the diaphragm gets electrical impulses from the pacemaker and starts. This can usually be resolved by replacing the electrodes
Any Questions?
Of course, if you have any questions or concerns, please discuss them with the ICU nurses and doctors.
All Intensive Care interventions and procedures carry a degree of potential risk even when performed by skilled and experienced staff. Please discuss these issues with the medical and nursing staff who are caring for your loved one.
The information contained on this page is general in nature and therefore cannot reflect individual Patient variation. It is meant as a back up to specific information which will be discussed with you by the Doctors and Nurses caring for your loved one. INTENSIVE CARE HOTLINE attests to the accuracy of the information contained here BUT takes no responsibility for how it may apply to an individual Patient. Please refer to the full disclaimer.
Related articles:
- How long does a cardiac arrest patient stay in Intensive Care?
- Six weeks in Intensive Care after Cardiac Surgery and my mother isn’t getting any better…
- How long can a breathing tube or an endotracheal tube can stay in?
- How long should a Patient be on a ventilator before having a Tracheostomy?
- How long is a Patient kept on a BIPAP machine in Intensive Care?
- What is an induced coma and why is my critically ill loved one in an induced coma?
- The 3 most dangerous mistakes that you are making but you are unaware of, if your loved one is a critically ill Patient in Intensive Care
- How to always achieve your goals whilst your loved one is critically ill in Intensive Care
- Why you must make up your own mind about your critically ill loved one’s situation in Intensive Care even if you’re not a doctor or a nurse!
- Follow this proven 5 step process on how to be in control and influential if your loved one is a long-term Patient in Intensive Care
- How to quickly take control and have real power and influence if your loved one is critically ill in Intensive Care
- Why does my loved one need a Tracheostomy in Intensive Care?
- Tracheostomy and weaning off the ventilator in Intensive Care, how long can it take?
- My sister has been in ICU for 21 weeks with Tracheostomy and still ventilated. What do we need to do?
- Severe lung failure and my aunty is not expected to survive…
- Be more selfish if your loved one is critically ill in Intensive Care
- How to stay positive if your loved one is critically ill in Intensive Care
- 4 ways on how to be more persuasive if your loved one is critically ill in Intensive Care
- 3 quick steps on how to position and prepare yourself well mentally, whilst your loved one is critically ill in Intensive Care
- How to get what you want whilst your loved one is critically ill in Intensive Care
- 5 steps to become a better negotiator if your loved one is critically ill in Intensive Care
- 5 Ways to have control, power and influence while your loved one is critically ill in Intensive Care
- How to make sure that your values and beliefs are known whilst your loved one is critically ill in Intensive Care
- How to make sure that “what you see is always what you get” whilst your loved one is critically ill in Intensive Care
- What the doctors and the nurses behaviour in Intensive Care is telling you about the culture in a unit
- How long does it take to wake up from a Traumatic brain injury or severe head injury
- How to take control if your loved one has a severe brain injury and is critically ill in Intensive Care
- Family Meetings in Intensive Care or the Elephant in the Room
- What you need to do if your loved one is dying in Intensive Care(part one)
- What you need to do if your loved one is dying in Intensive Care(part two)
- Intensive Care at its best?
- How INTENSIVECAREHOTLINE.COM Can Help You
- What you and your Family need to do if your critically ill loved one is very sick in Intensive Care and faces an uncertain future
- How long can somebody stay in Intensive Care?
- My Family can’t agree on what’s best for my sister in Intensive Care…Help!
- My husband is dying in Intensive Care, but we need more time…
- My mother sustained serious brain damage after a stroke and she now is in multi- organ failure


