What is abdominal trauma?
Abdominal trauma is an injury to the abdomen. It may be blunt or penetrating and may involve damage to the abdominal organs such as liver, stomach, kidneys, spleen, bladder, pancreas, intestines(bowels) etc…. Signs and symptoms include abdominal pain, tenderness, rigidity, and bruising of the external abdomen. Abdominal trauma presents a risk of severe blood loss and infection. Diagnosis may involve ultrasonography, computed tomography(CT), and peritoneal lavage, and treatment may involve surgery.Injury to the lower chest may cause splenic or liver injuries.
Abdominal trauma occurs when the structure and organs of the abdominal cavity are injured through falls, car accidents or deliberate acts of violence.
- The Abdomen
- Complications
- Treatment for abdominal trauma
- What Happens in Intensive Care?
- How long will your loved one remain in Intensive Care?
- Publishing Information
The Abdomen
The abdomen consist of the gastrointestinal system (stomach, liver, pancreas, and intestines), the renal system (kidneys), the spleen and arteries and veins including the aorta.
Source: Family Doctor UK
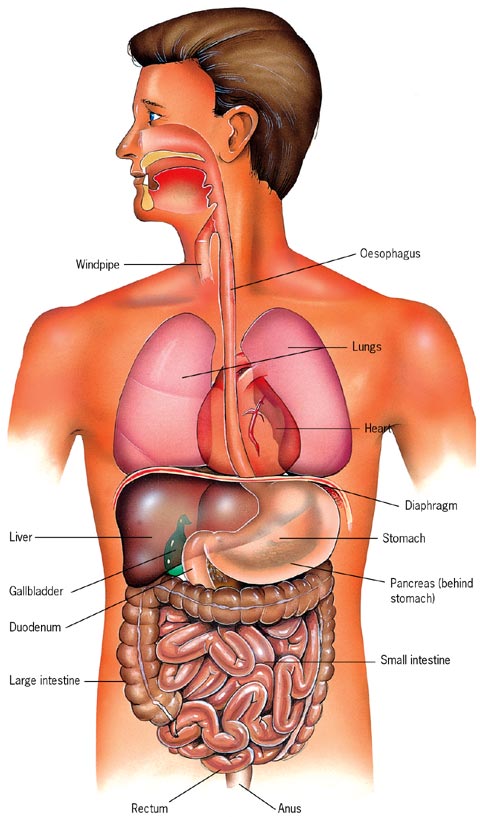
Penetrating trauma typically results in injury to organs in the direct path of the instrument or missile, but high-velocity weapons may cause injury to adjacent organs as well.
Treatment for abdominal trauma
Initial treatment involves stabilizing the Patient enough to ensure adequate airway, breathing, and circulation, and identifying other injuries. Surgery may be needed to repair injured organs. Suspected hemorrhage will be identified quickly using clinical assessment and an abdominal ultrasound. Chest and abdominal x-rays may indicate disruption of the gastrointestinal tract or may identify penetrating objects. Surgical exploration is necessary for people with penetrating injuries and signs of peritonitis or shock. Laparotomy is often performed in blunt abdominal trauma, and is urgently required if an abdominal injury causes a large, potentially deadly bleed. However, intra-abdominal injuries are also frequently successfully treated nonoperatively. The use of CT scanning allows care providers to use less surgery because they can identify injuries that can be managed conservatively and rule out other injuries that would need surgery. A range of blood tests will be done in Intensive Care.
There are a number of operations that may be performed according to the findings at operation. Below is a short list of common terms that may be of use.
- Laparotomy – an exploratory operation of the Abdomen where the surgeons look for problems and operate according to their findings.
- Laparoscopy – an exploratory operation of the Abdomen performed using key hole surgery.
- Splenectomy – removal of the spleen.
- Nephrectomy – removal of a kidney.
- Anastomosis – surgical procedure where two parts of the bowel are joined together.
What Happens in Intensive Care?
- Your loved one with abdominal trauma will be admitted to Intensive Care if they have suffered a severe injury. They may have experienced trauma to a number of other body areas (classified as multi-trauma). On most occasions your loved one will be admitted to the Intensive Care following surgery. Once in ICU your loved one will be under the care of the Intensive Care team with the surgical team reviewing your loved one on a regular basis.
- Your loved one is continuously monitored with a Bedside Monitors– Your loved ones vital signs such as Blood pressure is usually displayed continuously on the bedside monitor via an Arterial Catheter. Your loved ones Heart, Heart rhythm(ECG), temperature and breathing rate is continuously monitored and displayed on the monitor. Oxygen levels are continuously monitored by an oxygen saturation probe attached to the finger or to the ear. Furthermore oxygen levels are intermittently checked with ABG’s(Arterial Blood Gases), where blood is drawn out of the Arterial line and tested immediately via a Blood Gas Analyser.
- Your loved ones breathing will be supported by additional oxygen via an oxygen mask, however your loved one may be on a Ventilator (Breathing Machine) and have a Breathing Tube inserted into their airway. They will be receiving intravenous fluids via several intravenous cannula’s or Central Venous Lines(central line or CVC). A urinary catheter is used to monitor urine output and a Nasogastric Tubes will be used to rest the intestine if this has been injured or if your loved one requires ventilation. Anti-thrombotic stockings will be applied to guard against the development of a deep vein thrombosis (DVT) in the lower limbs. A sequential compression device may also be used. Pain medication will be given to ensure they are as pain free as possible. Nutrition will be started as early as possible. Feeding via a nasogastric tube is preferred. However if this is not possible, your loved one will be fed intravenously with TPN(Total Parenteral Nutrition).
Complications
- Hemorrhage can result in shock and complications associated with massive blood transfusions. Delayed hemorrhage from liver or spleen bruising tends to occur several days after the initial injury.
- Infection: intra-abdominal infection(Peritonitis) can be a significant problem. Predisposing factors include injury to the intestines, open wounds, delayed diagnosis of hollow organ injuries, and large amounts of damaged tissue.
- The stomach and intestines often fail to work for a variable time after injury. This causes problems such as delayed stomach emptying and paralytic ileus (paralysed bowels).
- Severe hemorrhage, bowel swelling or bowel paralysis can lead to a high intra-abdominal pressure as the fluid collects inside the abdomen. This can make it more difficult for your loved one to breathe because of increasing size and pain. Sometimes the pressure inside the abdomen may need an operation to reduce it and afterwards the surgeons use a mesh repair or leave the abdomen open. Repeated operations are required and the abdomen is closed in stages.
How long will my loved one remain in Intensive Care?
This is a difficult question to answer and all depends on your loved ones circumstances, determined by the initial injuries and subsequent complications. Please direct questions regarding your loved one to the intensive care and surgical staff.
Any Questions?
Of course, if you have any questions or concerns, please discuss them with the ICU nurses and doctors.
All Intensive Care interventions and procedures carry a degree of potential risk even when performed by skilled and experienced staff. Please discuss these issues with the medical and nursing staff who are caring for your loved one.
The information contained on this page is general in nature and therefore cannot reflect individual Patient variation. It is meant as a back up to specific information which will be discussed with you by the Doctors and Nurses caring for your loved one. INTENSIVE CARE HOTLINE attests to the accuracy of the information contained here BUT takes no responsibility for how it may apply to an individual Patient. Please refer to the full disclaimer.
Related Articles:
- How long can a breathing tube or an endotracheal tube can stay in?
- How long should a Patient be on a ventilator before having a Tracheostomy?
- How long is a Patient kept on a BIPAP machine in Intensive Care?
- What is an induced coma and why is my critically ill loved one in an induced coma?
- The 3 most dangerous mistakes that you are making but you are unaware of, if your loved one is a critically ill Patient in Intensive Care
- How to always achieve your goals whilst your loved one is critically ill in Intensive Care
- Why you must make up your own mind about your critically ill loved one’s situation in Intensive Care even if you’re not a doctor or a nurse!
- Follow this proven 5 step process on how to be in control and influential if your loved one is a long-term Patient in Intensive Care
- How to quickly take control and have real power and influence if your loved one is critically ill in Intensive Care
- Why does my loved one need a Tracheostomy in Intensive Care?
- Tracheostomy and weaning off the ventilator in Intensive Care, how long can it take?
- My sister has been in ICU for 21 weeks with Tracheostomy and still ventilated. What do we need to do?
- Severe lung failure and my aunty is not expected to survive…
- Be more selfish if your loved one is critically ill in Intensive Care
- 3 quick steps on how to position and prepare yourself well mentally, whilst your loved one is critically ill in Intensive Care
- How to get what you want whilst your loved one is critically ill in Intensive Care
- 5 steps to become a better negotiator if your loved one is critically ill in Intensive Care
- 5 Ways to have control, power and influence while your loved one is critically ill in Intensive Care
- How to make sure that your values and beliefs are known whilst your loved one is critically ill in Intensive Care
- How to make sure that “what you see is always what you get” whilst your loved one is critically ill in Intensive Care
- What the doctors and the nurses behaviour in Intensive Care is telling you about the culture in a unit
- How long does it take to wake up from a Traumatic brain injury or severe head injury
- How to take control if your loved one has a severe brain injury and is critically ill in Intensive Care
- Family Meetings in Intensive Care or the Elephant in the Room
- What you need to do if your loved one is dying in Intensive Care(part one)
- What you need to do if your loved one is dying in Intensive Care(part two)
- Intensive Care at its best?
- How INTENSIVECAREHOTLINE.COM Can Help You
- What you and your Family need to do if your critically ill loved one is very sick in Intensive Care and faces an uncertain future
- How long can somebody stay in Intensive Care?
- My Family can’t agree on what’s best for my sister in Intensive Care…Help!
- My husband is dying in Intensive Care, but we need more time…
- My mother sustained serious brain damage after a stroke and she now is in multi- organ failure


