Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
My Brother is Not Waking Up in ICU. So What’s their Plan in Getting Him Out of the Induced Coma?
You can check out last week’s question by clicking on the link here.
In this episode of “YOUR QUESTIONS ANSWERED” I want to answer a question from one of my clients Megan, as part of my 1:1 consulting and advocacy service! Megan’s brother is ventilated in ICU with pneumonia and the ICU team issued a DNR status for her brother without her consent. Megan is asking what she should do.
My Brother is Ventilated in ICU with Pneumonia and the ICU team Issued a DNR (Do Not Resuscitate) Status for Him Without My Consent? What Should I Do?
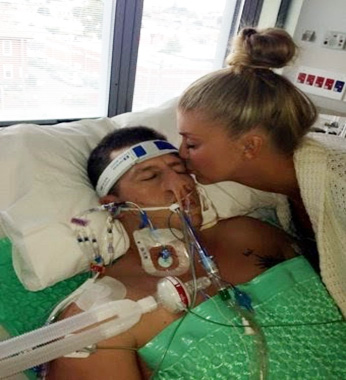
“You can also check out previous 1:1 consulting and advocacy sessions with me and
Patrik: Okay, so it’s basically, 24 hours. So if it’s 24 hours, they should hopefully, have a better idea after they’ve done an X-ray and even this morning, he would’ve had an X-ray, chest X-ray. So even then, they would have an indication of what the chest X-ray today looks like, compared to yesterday, compared to the day before and so forth. That’s a really good indicator of where he’s going.
Megan: Okay.
Patrik: So then, do you know how much noradrenaline he’s on? Do you have a number? Yeah. And you know what you could also get? You could also get a picture of the ventilator if you can. Look, I think at the moment, from what you’re sharing, I really think it’s way too early to see where this is going. And obviously, panic is the worst thing you can do. The most important thing really is just to stay calm and stay collected. That’s really important. And just to be prepared that…
RECOMMENDED:
Patrik: You see, from experience, and you would’ve seen it probably with your parents, as soon as there’s the slightest sort of deterioration, they’re going to be even more negative and it’s all going to be doom and gloom. And it’s really important for you to put things in perspective and not buy into this negativity. What I always say is the worst-case scenario, from an ICU perspective, are they’re looking after a patient indefinitely, with an uncertain outcome. That’s the worst case scenario for an ICU. Right? And the minute there are signs that this worst-case scenario for them could unfold, they’re becoming extremely negative.
Megan: Yes, you’re right.
Patrik: Yeah, sure. Yeah, look. It is very early days, but the most important thing is that you are prepared for this because you’ve seen it before, you’ve now, get the insights from me as well, in terms of if there’s any sort of… they ask you for a family meeting and they can’t be quick enough, you just put the brakes on. You put the brakes on and very few families do that, but if I guide them and I say, “Look, you put the brakes on,” I have not seen anything bad happening because they know that they have a duty of care for your brother, as well as towards you. Right. And they can’t just withdraw treatment without talking to you, without… The sad thing in Northern Ireland is that they don’t need to consent to you, but they need to consult you.
Megan: Yes at least inform and consult us.
Patrik: But at the same time, if you feel like they’re going to withdraw treatment and we think there is evidence that there is every reason for hope… Right? That’s when… That’s right. That’s exactly right. And also then, question, in regards to… We need to question then, have they done everything within their power? Are there things they could be doing? Are they doing… Could they potentially, refer to another hospital? It’s all those questions that will need to be asked then. But I can’t see, at the moment, with the information you’ve shared, there is no reason to be negative.
RECOMMENDED:
Megan: Alright.
Patrik: Just going back to Alfie Evans for one moment. Some of the agenda for Alfie Evans family was driven by the Catholic church. Now I can tell you, I’m not Catholic by any means and you don’t need to be a Catholic to be, what I believe, a decent human being and to be a problem-life. You don’t need to be Catholic, but what’s happening there in Northern Ireland, I just go like, “This is horrendous.”
Megan: Yes I also feel like that.
Patrik: I’m German by background, and I can say, some of what’s happening there is like the Nazi-style. I can’t believe it; what’s happening there. Unbelievable. Right. Terrible. But there’s another element of that, which is one of the reasons why I started doing what I’m doing. I have felt, when I was still nursing at the bedside, there have been numerous situations where I felt compromised in my beliefs, in my ethics; where I just said, “Hang on a sec. I’m not doing this. You can sack me. I don’t really care. You can sack me or whatever. I don’t really care.
Patrik: Because I was at the point where I just thought, “No, I’ve got to find another way to earn a living and I’m just not doing that.” And what I learned there then was… or what I’m still seeing, and again, I keep going back to Alfie Evans but also, other… I can’t believe that there is a nurse or doctor carrying out what they carried out. That is the most frustrating part to me; that there is an individual carrying out what a government or a court decides. Yes, some of it is obviously wanted by the medical fraternity, but there is still an individual; whether a doctor or a nurse, on the other end, carrying out what is against families’ wishes. And I just got… I came on, I said, “Why did you become a doctor? Why did you become a nurse?” That is the most disturbing part for me.
Megan: I can’t believe it myself as well that they have to do like that.
Patrik: It’s brainwashing and it’s also like hospitals being political hierarchical. And some, whether it’s doctors or nurses, they might follow through because they think, “Oh, maybe there’s a promotion for me on the other end.” That is the disturbing part. That is the disturbing part. Yes, and that’s not going to happen. And that’s something that I learned because I was at that point. I learned that I wasn’t losing my job because I had everything lined up, in terms of, “Look, here is my nursing registration, here is my code of conduct, here is my code of ethics. I’m just following that.” And that, to me, is disturbing that the nurses or the doctors… It doesn’t matter whether they’re doctors or nurses, I’m not referring back to the authorities, which you can. And the authorities are actually not that bad. The nursing board would back you up.
RECOMMENDED:
Megan: Okay. Being a good ICU nurse takes a lot of courage and good disposition I believe.
Patrik: Oh, very much so. Very much so. Very much so. Courage and… but also, it takes years of experience as well to understand. When I was new in ICU, I had a different set of eyes than I have now of course, right? I didn’t see, in the first five years of ICU, what I see now. Right. That comes with time, with practice, with experience. After 10 years of ICU, I had a very different view. Right. Because then you understand the politics. You understand what’s really driving treatment, research, whatnot. Then you understand the whole machinery, which I didn’t… In the beginning, you’re just learning the clinical things. You’re not looking at who’s making the decisions in the background. Yeah, you can’t.
Megan: Yes I agree with you.
Patrik: And I can tell you, even with what I’m doing now, I’m doing still, two shifts a month in ICU to keep my fingers on the pulse, right? And I have not… Despite how I’ve positioned myself in this environment, I have people… If anything, I think people respect me. It’s not a secret what I’m doing. A lot of people know all the crap that’s happening and they don’t necessarily agree with either. So I have not found that there was any animosity or… because yeah, it’s just what it is.
Patrik: The reality is that after 20 years of ICU, the reality is that people move away from it anyway because it’s a high-stress job, shift work, weekends, the whole… So people move away from it, not necessarily because they’re frustrated, probably because they’re burned out because it’s hard work.
Megan: It must be really difficult.
Patrik: It’s okay if patients go in and out. If there’s a quick turnover, it’s not too bad, but especially for long-term patients, imagine you’re confined for weeks or sometimes for months, with no natural daylight. It’s terrible. Yes, it is like torture; absolutely. Very much so. But with what you’ve shared there’s no need to panic at this point. I tell you what you might want to look for and you might have brought it up already, if your brother was on medications for his bipolar before he went into the hospital, the waking up could be a challenge if he’s of those medications. Why? They said that? Okay, good. But why is it a challenge? Most patients coming out of an induced coma are confused, to begin with. So imagine you’ve got the added on layer of complexity of a bipolar disorder.
RECOMMENDED:
Megan: Yeah. I got that.
Patrik: So there could be some challenges, but it doesn’t necessarily have to be a challenge. I’m just saying it could be. Look, they can be addressed but the reality is that if he’s to wake up and he’s confused, often they address it with more drugs, which I believe will make him more confused. That’s my experience. I don’t know. Have you heard of the drug, for example, haloperidol? It’s sort of a standard drug used in ICU for confusion and I believe it’s making things worse.
Megan: I think it’s important for me to ask them that and I need to take note of all of this. This would really help me a lot in terms of what are the right questions to ask them.
Patrik: Yes. Just quickly, summarizing a few pointers. I can send you the recording of this phone call if you like. And I will just make a quick, few pointers of what you should be asking. But there is absolutely no point in panicking at the moment. It’s just being mindful of how you behave with them; especially if you feel like, “They’re going down that negative track,” or doom and gloom.
Megan: Yes I know I need to know how I should respond to them.
RECOMMENDED:
Patrik: And what I’ll do next, I will send you a link to that. I will credit this hour towards… So I will send you a different link anyway. You are out of your depths because there’s so much specialized knowledge; not only clinical knowledge, it’s mainly what’s happening really, behind the scenes, in terms of what do they come forward with that they probably discussed five minutes beforehand, to line you up for something that would shock you and your brother of course. And your brother may never find out. So it’s that sort of thing; to be prepared for the worst-case scenario.
Megan: Okay. I should better be ready for that.
Patrik: And let me ask you this. Is there any other medical history besides the bipolar? There’s no kidney failure? I tell you what you need to ask for and I’ll put it in the email. You need to ask for the renal markers or the kidney markers in the blood but as well as asking is he making urine. Do you know whether he’s making urine? Okay, all right. Okay, that’s good. That’s good. Right. So it’s just a matter of asking that. That’s all you can do for now.
Megan: Yes, my brother is making urine, clear that is. And I think they are monitoring his urine output as well.
Patrik: Yeah, they would have a baseline for his kidney markers and they would watch that every day. And they would watch that every day and they would obviously monitor his urine output. There is also a chance that… especially when you’re saying he’s got really clear urine, there’s a very good chance they’re giving him furosemide for the simple reason that anybody with pneumonia, you want the lungs dry. Any excess fluids on the lungs could delay clearing pneumonia, could delay getting somebody off the ventilator.
RECOMMENDED:
Megan: Yes, I think I have heard that they are giving him that medication.
Patrik: So there’s a very good chance that they’ve given him furosemide to keep him dry, to minimize the fluids on the lungs. And that would then, make his urine look very clear. A little bit of furosemide in pneumonia is almost part of a standard pack because of the reason that I mentioned.
Megan: Oh I see. Thank you for all this information. It really helps a lot.
Patrik: I’ll send you another email just with the options down the line if you want that; the four and the seven-day option. And then you can take it from there. But because you are now a member, I also answer your daily emails. If you don’t want to get on the phone, just for being a member, I will answer your daily emails as well. Yeah, there’s a chat room where you can contact me or you can just send me an email; either is fine. Not so much. It’s relatively new. It’s relatively new. You are the third subscriber, I can tell you that much, for the membership. So therefore, there is not a lot of activity in there. And that’s why I’m saying if you want to send me an email instead, that’s absolutely fine.
Patrik: I’ve also refunded the e-book that you purchased yesterday. You’ve got the e-book of course because you have access to all of the e-books in the membership. Right. But as I’ve said, if you want the four or seven-day option, that’s absolutely fine and then you have access to me over the phone of course. If you want to continue the conversation via email, that’s absolutely fine.
Megan: Ok. Thank you for your time.
Patrik: You’re very welcome. Thank you. Have a good day. Bye.
Megan: Bye-bye.
RECOMMENDED:
Megan: Hello Patrik.
Patrik: Hello Megan. How are you?
Megan: Hello there. I’m not too bad. Still struggling on. And you?
Patrik: I’m very well, thank you. I’m really well. Thank you.
Megan: Good, good.
Patrik: I’m worried about the ongoing battle.
Megan: Yes, honestly. And isn’t it ironic I got in? Because there hadn’t been much going on. It was just going on much the same, and “I must give you that email,” I said. And then literally the next day, they pounce on me.
Patrik: I shouldn’t have even said that but I, I just see it so often. I didn’t want to jinx it or anything, but I’ve seen it so often.
Megan: Yes, it was … and the other thing that was so clever is that it didn’t say the doctors want to see you, then it would have alerted me. I could’ve got my thoughts together. They literally pounced on me. They pounced and closed the curtains and he sat in front of me and he got me in the corner and I couldn’t even get out.
Patrik: Guerrilla tactics.
Megan: Guerrilla tactics, and he was saying things, and Ryan can hear and he was saying these things. Why next to Ryan as well? I don’t know why he was doing that.
Patrik: So inappropriate. So basically, he was saying the things that you put in the email in front of Ryan?
Megan: He was saying, he didn’t say the thing about we hope he has a heart attack. That was this other ghastly woman. She said, “I hope he has a huge blood clot and a huge heart attack and he just dies.” And I put-
Patrik: So inappropriate.
Megan: … So nice. So inappropriate. She can think that she can think it, but, and then so she said, so I’m putting DNR on so if that happens, then it happens.
Patrik: So she issued a DNR?
Megan: Yeah, she did it the next day.
Patrik: Have you had a say in that?
Megan: Nope. They won’t let me.
RECOMMENDED:
Patrik: So how long ago-
Megan: She said, “It’s not up to you.” She told me. It’s not up to me. “You don’t ask your permission,” she said.
Patrik: … How long ago was that?
Megan: That was when he first went in, which was a long time ago now, which was the 4th or let’s see. He went to the hospital on the 30th, he went into the ICU on the 4th of August. So we’re coming up to that period of time where they start to lose interest I think.
Patrik: I can’t look, with all of our discussions, I can’t remember us talking about DNR. The reason I, because I’m sure if we had talked about this before, I’d tell you my thoughts on that. I mean, let me ask you this, do you agree with that?
Megan: No.
Patrik: Okay. If you were to ask Ryan, would he agree with that?
Megan: No.
Patrik: Right. Okay. So then I’ll tell you the next steps if you want to. So you could go back to them and say you want to see the hospital policy around DNR. So the reason for that is, she’s telling you that they don’t have to get your permission. However, that’s what she’s telling you. Whether that is in line with their hospital policy, I question.
Megan: Yes.
Patrik: Right? So it really depends on how confrontational you want to be.
RECOMMENDED:
Megan: I want to be.
Patrik: Yeah, no, I think so. Look and are you … all you’ve got to say is, “Well, please give me the hospital policy about DNR,” and then you will see how they react. And you can, if they ask you why, number one, you don’t have to tell them why. But number two, you can tell them, “Well, because I don’t agree with the DNR.” And number two, what’s probably even worse is there would have been a period in all of this, they could have asked your brother, couldn’t they? What he wants. It’s bad enough that they tell you that they don’t have to ask you, but I think it’s even worse than they haven’t asked Ryan.
Megan: Yes. I mean they put it on, she put it on when they had … so he went in and they put him on the hood, and then very quickly thereafter they intubated him. Obviously, at that point, he was heavily sedated, and that’s when yeah, she kind of swooped … The consultant that’s on today, but he finishes today, is completely different in his attitude to the one that I saw two days ago. He said, “But let’s hope we can bring him on. I can’t promise you, and he won’t be the same, but let’s hope. We just have to hope that he can just turn that corner, or we can get him onto the back to the ward.”
Megan: That’s what the good doctor said. And get him home. And he said it will probably be three or four months of rehabilitation at home, as long as you understand all that, we don’t continue obviously, but let’s just hope he can turn the corner. And then this one says, “He’s going to die.” Two days later, it’s very bizarre.
Patrik: Yeah. But you were also saying something in this email, which I think is really important. You said, and again, I kind of giggled here, which I shouldn’t, but you were saying they had a meeting.
Megan: Yes, they had a meeting.
Patrik: And then it all changed.
Megan: And then it all changed. We went from, “Let’s hope he can get home. Let’s hope he can do it” to, “He’s going to go, he’s not going to make it.” After the meeting, you know Patrik, I know from your videos and your literature and your website, everything, that it’s these meetings that are the deadly time, this is when they get together and decide the state of your loved ones.
RECOMMENDED:
Patrik: Very much so. Very much so.
Megan: That’s why you’re giggling because I do know Patrik, you’ve seen that too many times. And the other thing is, I only found that out from the nurse. Because I said to the nurse, “Well, that was,” because she closed the curtains and then the consultant went. He was very unpleasant. And I said to her, “That’s a bit of a change, isn’t it?” And she suggests they had a consultant’s meeting and they, so they all say what they did. So, there we go.
Patrik: So the nurse knew as well. This was after consultant meetings.
Megan: This was directly after. He literally sat down and he just looked me straight in the eyes and he said, and he said it in a most unpleasant way. He said, “Ryan’s not going to make it.”
Patrik: And that was in front of Ryan?
Megan: Ryan.
Patrik: That is so inappropriate. And Ryan was awake at that point in time?
RECOMMENDED:
Megan: Well, Ryan had the radio. I’ve got Ryan a radio to try and give him some comfort and ground him a bit. That there is life outside this terrible place. I cannot tell you whether he heard or not, but if I say, Ryan, he’ll open his eyes and look at me. So I think he may very well have heard.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!