Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
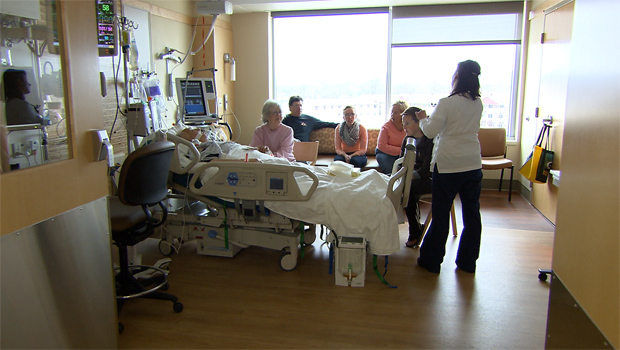
Hi, it’s Patrik Hutzel from “INTENSIVECAREHOTLINE.COM” where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from one of my clients and the question in last week’s episode was
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED“, I want to answer the next questions from one of my clients Natasha stating that documentation has not been done during the last hours of her Dad dying in the ICU.
I always heard my intubated Dad in ICU gargling and the ICU staff said it’s just ok. Is he at risk for aspiration?
“You can also check out previous 1:1 consulting and advocacy sessions with me and here.”
Natasha: They wrote down the cuff pressure.
Patrik: But that was only once. It needs to be written down at once the shift. Three times.
Natasha: No it was. It was. It was written down. The cuff pressure was written down for every time they checked it, they did write it down every time. But what I’m saying is that, all of a sudden it was from March 31st until April 4th, early during the day, his endotracheal tube was a 24 centimetres and tight cuff pressure and it was chest with the capnometry, whatever device that is. But then, after that, they stopped checking with the capnometry device and his endotracheal tube was now secured at 23 centimetres and the cuff pressure was 22. But there was no capnometry confirmation. But they did write that down. So my whole thing is that it changed. Like it shifted his whole, but they did write it down. But what I’m saying is what effect did that have on him and …
Patrik: Okay, well the effect is that-
Natasha: That it’s up?
RECOMMENDED:
Patrik: Yeah. Especially with the gargling. You said you heard the gargling more than once, haven’t you?
Natasha: Yes, a lot. A lot.
Patrik: Yeah, so that’s why so important. If number one, there is gargling, okay well the first question to me is, is there a cuff leak? Okay so number one, either a nurse or respiratory therapist, they need to check the cuff pressure, okay. And then they obviously need to document but also need to make sure there’s no more gargling. Now if there is gargling even though they increased the cuff pressure, they then need to go back to the doctor and say, “Hey, do we need to change the ET tube?” That’s one thing.
Natasha: Yeah, that’s one thing.
Patrik: Yeah. None of that probably in the notes. As I said, I’ve only glanced over it. So the next question is-
Natasha: And no they didn’t do that. They just said that it’s okay for him to gargle.
Patrik: No it’s not. I can tell you it’s not.
Natasha: Yeah, I know it’s not.
Patrik: And so then the next question is okay, risk, we mentioned that, risk of aspiration. And number two is, is he getting all his target volumes? How does that impact on his ventilation? Because with the leak, basically what happens is if they’re ventilating him with whatever, this 500 mls per breath, he might not get that 500 mls because of the leak.
Natasha: Yeah.
Patrik: Right?
Natasha: Yeah.
Patrik: And again those are all the things that we can find out. Now I can tell you because I looked, I glanced over the 1,200 pages. To give you a rough idea-
Natasha: Patrik can I talk to you really quickly about that? But then another thing is what, there’s some things they didn’t write correctly in the notes though. They could just lie about some of this stuff though, because some of this stuff was not correct.
RECOMMENDED LINKS:
Patrik: Yes. They could like about this stuff. I mean that risk is always there. But I guess that’s where our specialised knowledge is coming in, where we can say, okay. Well, okay, so I’ll give you an example so you can put this in perspective.
So let’s just say there was gargling and they didn’t document that. And there’s somewhere document says oh yeah everything has been fine.
Natasha: They haven’t.
Patrik: But one thing is in there for example is the ventilator parameters. So you know there’s definitely enough information in there about what his ventilator settings were, also what his blood gases were. So we can look at, for example, what he has been ventilated on, number two what the blood gases has said, what other vital signs have been, right? Whether that’s all correlating.
Natasha: Yeah, I see. So it’s not just one thing. You can’t change. They can’t falsify everything.
Patrik: No, no, no, no, no, no. No. No. It’s everything. And that’s why I think it would also be worthwhile of maybe getting some chest x-rays, some films. But you know, up to you how you want to go about it. But just because I had a look at this now-
Natasha: I’m gonna have to find a way to copy it, yeah.
Patrik: So hang on. With the chest x-ray films, have you got them on software or how do you …?
Natasha: Okay, so let me look at them. I have it right here, hold on. It is on … they gave it both to me on a disc. So it is on a CD-ROM. A DICOM. A DVD. And, yeah. So I guess I have to bring it to like Staples or something and just have them make a copy?
Patrik: Right.
Natasha: See if they can just do that.
Patrik: Right. Okay.
Natasha: And then …
RECOMMENDED ARTICLES:
Patrik: Right okay. So what you can do then is most likely you can copy that onto your google drive or whatever you, yeah you can copy to google drive and then you can share it on google drive. It should be as simple as that.
Natasha: Yeah, I guess I can do that. I just didn’t know how to. I guess I can just do it that way. Okay. Okay.
Patrik: Okay, so look. To give you an estimate now, just by looking at this. As I said to you, we have reviewed, or we are reviewing notes of other clients too. And I say from my perspective, rather than charging by the hour, I would rather quote you a flat fee for this and given the amount of notes, I would think, probably around $900.
Natasha: Okay, I would, stuff like that ’cause it’s a lot.
Patrik: It’s too much. It’s too much in terms of notes. It’s not … I was expecting maybe two or 300 pages and then … but 1,200 pages that’s massive.
Natasha: Yeah. Yeah I feel like, because the amount that he actually had when he was first in the hospital, I don’t know, from his whole hospital stay, it’s a lot for one week.
Patrik: It’s a lot. It is massive.
Natasha: Okay. All right. Okay. And then you have your PayPal thing.
Patrik: Yes, it would go through via PayPal. And then you would get a report. And what we could go also do as part of this whole package, what I would consider a package, you will definitely get a conclusive report. But you could then, if you wanted to, you could then either follow up with another Skype call if you have any questions obviously with either myself or the person who’s going to review the notes. Probably even with the person who’s reviewing the notes.
Natasha: Yeah. Yeah, sounds a good idea.
RECOMMENDED INFO:
Patrik: Right?
Natasha: Yeah.
Patrik: I mean I’m sure you would have a lot of questions. Before we proceed, it’s up to you, I can send you a paper link once we come off this call, but you gotta think, do you want to go ask the hospital about more notes or do you just want to go with what we’ve got? What’s your feeling?
Natasha: No, I do want to get more notes. I’m trying to figure out how I can ask them for … without … ’cause I don’t want them to be like, “Oh…” ‘Cause I think that they just knew that it was me calling. Like they knew, they knew that it was me.
Patrik: You know what you could do, there must be, besides … now there’s some scratching, I can barely hear you. There’s some scratching going on in the background.
Natasha: Yeah, I know the Skype is bad, let me call you back.
Patrik: Okay.
Natasha: Can you hear me?
Patrik: I can hear you, can you hear me?
Natasha: Yes, I can hear you good. Okay.
Patrik: Okay, the other way to go about it might be … They must have a patient liaison type of office.
Natasha: Yes, it’s the patient relations office.
Patrik: Oh yes, yes, something like that. Have you spoken to them?
Natasha: Yes, when you were there I would … That’s another thing, the complaints I’ve filed, well, I didn’t do anything formal, but they didn’t send me any of that. But yes, that’s the person who called me from patient relations, “Do you have any questions about your father? Please contact us, blah, blah, blah.” And so I was actually waiting to hear back. I wasn’t sure, should I ask … I didn’t want to call her back until I spoke to you or my sister, because I didn’t know how to approach it. Because, I know there’s things missing, and I didn’t know how to ask, but I need that information, so just ask her, what, politely, I mean, try?
RECOMMENDED LINKS:
Patrik: Yes, just ask her politely. You know, the one thing, I’m just trying to think, I am certain there must be some notes in relation to nursing documentation. There must be, right? The nurses have to cover themselves just like the doctors have, with entries, right?
Natasha: I saw them, too. I would see them typing in … I know I saw one nurse doing that, actually typing a note about my dad, like about what she did or something. She was kind of polite, she was kind of nice to me. Then, I went up to her and talked to her, and I remember I did see her typing something, and she was talking out loud about my dad. I didn’t see any entry like that, so I don’t know. I don’t know what happened.
Patrik: Right, and did you, for example, see at the bedside they’ve had folders or files with paperwork?
Natasha: No, by the bedside? No.
Patrik: Right, right, because that would be my first guess, you know, that if somebody is doing a manual entry like a handwritten report, that they would have a file or a folder at the bedside with paperwork.
Natasha: No, I never saw anything like that. No.
Patrik: Right, I can’t believe that there is no nursing records whatsoever. You know, that that’s just not-
Natasha: It’s all about me.
Patrik: Oh, I looked … They mentioned you here.
Natasha: Me being emotional, that’s about it, the nursing notes.
Patrik: But, that’s doctors’ notes. I thought-
Natasha: No, it is, but some of blurbs, like do you see the plan of care, they write about how, “Daughter is so unrealistic.” Just bullshit, nothing to do with what’s going on.
RELATED INFO:
Patrik: Agreed, agreed.
Natasha: Just nonsense, like they’re documenting nonsense, and attributing things that I didn’t even say.
Patrik: Yes, yes. Agreed, agreed.
Natasha: Okay, so missing, yes, nursing notes I know, and then the films as well, okay.
Patrik: And the films, yes.
Natasha: And the research study, I have also that … Because, I ran through some of the medications with my sister that my dad was taking, and they were giving him steroids, right? And I remember they had to cut down his steroids to half, because something that I think something with tachycardia. I don’t know how to say that word.
Patrik: Yes, tachycardia. Yes.
Natasha: I don’t know what it … Yes, tachycardia, and I think they were giving that for his COPD, and they’re also giving him Pulmicort-
Patrik: Yes.
Natasha: On top of Albuterol.
Patrik: Yes.
Natasha: So, they were giving him a few things, and then my sister asked, “Were they giving him the steroids as part of the experiment? Because they shouldn’t be doing that, because that can cause fungal infections and it can mask infections. What the hell were they doing?”
Patrik: Absolutely.
Natasha: She asked, “Why the hell were they doing that?”
RECOMMENDED INFO:
Patrik: Yes, I totally agree with you that they shouldn’t have given any steroids. From our perspective, there’s no indication why he would’ve needed steroids. But again, I haven’t looked at it in detail. It could’ve well been part of the study, so I guess the question that you need to ask is do you need … You probably should get something from the study if you can, and number two, nursing notes. There must be something. I mean, that’s …
Natasha: It has to do with so much action. Patrik, literally, that last hour when all that action was happening, right, with my dad, that last one and a half hour, nothing, no nursing notes, nothing. All it is, is that Dr. Sharma writing that little blurb in his progress notes. Literally, no nursing notes about … Remember how I told you how it all went down? Like, this part, nothing, and the vitals were all off. They really found that his oxygen at 89, no, he was going down in upper 50s and 60s. Then, one note was like, “50,” and then everything else was … They just stopped documenting it properly in the end, the most important part.
Patrik: Yes, yes. So yes, as I said, I have not seen that there’s no nursing notes. I just haven’t, and from what I’ve seen just by glancing over the notes, not reading in detail, the respiratory therapies, I believe there is some notes from them here and there. But, from what I’ve seen, it’s not consistent.
Natasha: Yes, it’s not. No, you’re right. It’s just, yes, it’s intermittent. Yes.
Patrik: The doctors’ notes are consistent from what I’ve seen, they are consistent.
Natasha: Yes, they are.
Patrik: There need to be consistent nursing notes too.
Natasha: Yes, I agree.
Patrik: And that just can’t go missing, it just can’t.
Natasha: Have you had other patients like that, or …
Patrik: Sorry?
Natasha: Have you ever had other patients who had that happen, where you got their file-
Patrik: No, no, no, and I’ll tell you why, I’ll tell you why: Okay, let’s just say you report a nurse to the nursing authority in your state. You might file a complaint towards the nurse in your state, you can do that. Okay, but with the nursing registration board. Okay, or you could make a complaint against a doctor. It doesn’t matter. You could make a complaint against anybody who’s a registered health practitioner, okay. If you do that, and you might say, “Hey, on April 5th, that nurse has done this, this, and this, and I think she violated my dad’s …” whatever.
So, that nurse has no … In this situation, from what we know now, if you did that, that nurse has no documentation to defend themselves. That’s why it’s so import … It’s also a matter of having some evidence, what a nurse has done during their shift, and that they’ve done everything that’s, quote unquote, “in the best interest for a patient”. Right, so that’s why the hospital can’t just … So, I am wondering, are they hiding something? I don’t know. But, it’s a possibility.
RECOMMENDED:
Natasha: Because, Patrik, I really went in on them. I told them, “I’m definitely going to complain about this place. I really, I cursed them out to the point … It got really bad, and then when you tell people that you’re going to do that and do this, and then that phone call, they know that maybe that, “Oh, my God. I hope she doesn’t do something like complain,” or, “We should just be ready to cover our asses,” or something. I don’t know. Okay.
Patrik: Yes, so that’s what I would do, to ask them, “Oh, there must be some nursing notes?”
Natasha: Yes, be polite.
Patrik: Yes, polite, and I’m just trying to find out … I’m just trying to think.
Natasha: Never run into this problem.
Patrik: Yes, yes, because I’m almost certain that they’re trying to hide this from you.
Natasha: I know, yes.
Patrik: For whatever reason.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!