What is Coronary Artery Bypass Graft(CABG) Surgery?
Coronary artery bypass surgery, also coronary artery bypass graft (CABG, pronounced “cabbage”) surgery, and colloquially heart bypass or bypass surgery is a surgical procedure performed to relieve angina and reduce the risk of death from coronary artery disease. Arteries or veins from elsewhere in the Patient’s body are grafted to the coronary arteries to bypass atherosclerotic narrowing and improve the blood supply to the coronary circulation supplying the myocardium (heart muscle). This surgery is usually performed with the heart stopped, necessitating the usage of cardiopulmonary bypass; techniques are available to perform CABG on a beating heart, so-called “off-pump”(OP-CABG) surgery.
- What does the cardiovascular system do?
- Poor or abnormal function
- Symptoms
- What happens in the Intensive care unit?
- How long will your loved one remain in Intensive Care?
- Internet Links
What does the cardiovascular system do?
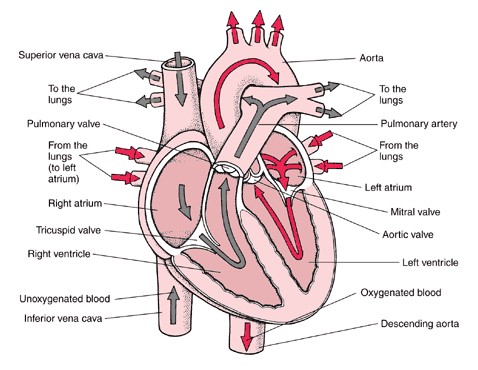
The essential components of the human cardiovascular system are the heart, lungs, blood, and blood vessels. It includes: the pulmonary circulation, a “loop” through the lungs where blood is oxygenated and the systemic circulation, a “loop” through the rest of the body to provide oxygenated blood. An average adult contains five to six quarts (roughly 4.7 to 5.7 liters) of blood, accounting for approximately 7% of their total body weight. Blood consists of plasma, red blood cells, white blood cells, and platelets. Also, the digestive system works with the circulatory system to provide the nutrients the system needs to keep the heart pumping.
The heart is at the centre, basically distributing blood from the ‘central pump’ with the blood vessels the pipes of the body, trying to reach every corner of the body. The cardiovascular system also passes nutrients (such as amino acids, electrolytes and lymph), gases(Oxygen and Carbon Dioxide), hormones, blood cells, etc. to and from cells in the body to help fight diseases, stabilize body temperature and pH, and to maintain blood pressure.
In the heart there is one atrium and one ventricle for each circulation, and with both a systemic and a pulmonary circulation there are four chambers in total: left atrium, left ventricle, right atrium and right ventricle. The right atrium is the upper chamber of the right side of the heart. The blood that is returned to the right atrium is de-oxygenated (poor in oxygen) and passed into the right ventricle to be pumped through the pulmonary artery to the lungs for re-oxygenation(inhalation) and removal of carbon dioxide(exhalation). The left atrium receives newly oxygenated blood from the lungs as well as the pulmonary vein which is passed into the strong left ventricle to be pumped through the aorta to the different organs of the body.The left side of the heart then receives oxygen rich blood from the lungs and pumps this blood into the Aorta and arteries of the body. This pumping action is a complex well-coordinated activity that cannot be fully explained here. The heart itself, receives oxygenated blood supply via the left and right coronary arteries.
Poor or abnormal function of the cardiovascular system
May be a result of:
- Insufficient blood supply due to dehydration, bleeding or swelling;
- A poor blood supply to the heart, where there is not enough oxygen and other nutrients for its work;
- Poor lung function or obstruction to blood flow in the lungs, which places a strain on the heart muscle;
- Too many or too few electrolytes (eg. potassium, magnesium) that cause irregular heartbeats or dangerous rhythms in the heart.
- Weakness of blood vessel walls.
- Heart muscle weakness Cardiomyopathy
- unhealthy lifestyle such as alcohol consumption, smoking, unhealthy eating habits, Diabetes and obesity
Symptoms
- Shortness of breath, Chest pain/heaviness, especially after exertion
- Pain in the shoulders, arms, neck or jaw
- Excessive tiredness
Management of these symptoms with medication may help in the short term, however it does not treat the diseased arteries. There is a high risk of a heart attack(myocardial infarct) occurring at any time, through the formation of a blood clot or thrombus, thus blocking the coronary artery, with a lack of oxygen supply to the heart muscle, leading to irreversible damage of the heart muscle. Coronary artery bypass grafting aims to restore the blood supply to the heart muscle, ideally at the stage when the artery is narrowed, and before the infarct occurs.
There are three main coronary arteries:
- Left anterior descending artery
- Circumflex artery
- Right coronary artery
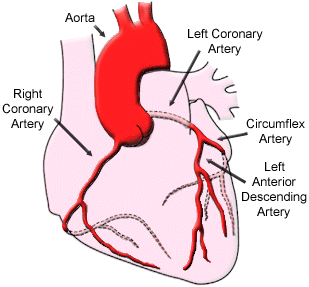
This picture was sourced from heart.org
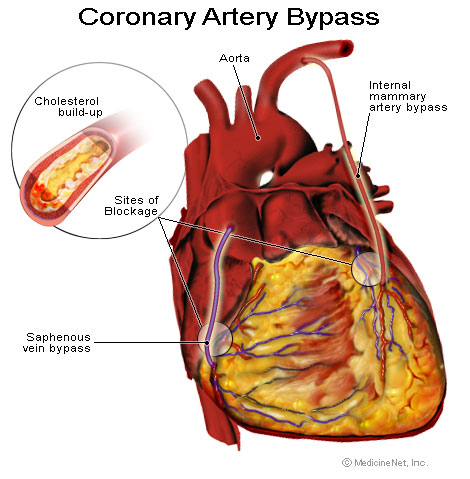
This picture was sourced from MedicineNet
What happens in the Intensive Care Unit?
- After coronary artery bypass surgery your loved one is admitted to the Intensive Care Unit.
- Full ventilation using a Ventilators(Breathing Machine) and a Breathing Tube (endotracheal tube) will usually be required for up to 24 hours after surgery to improve and maintain the oxygen delivery, as your loved one is usually unable to breath for themselves immediately after surgery. The ventilator is usually “weaned off” over the next 12-24 hours, sometimes even quicker, after ensuring haemodynamic stability of your loved one is achieved. The process of weaning somebody off the ventilator my take longer in a Patient with lung disease
- Sedation may be used for ventilator tolerance and if your loved one is in an induced coma. Common sedation used is Propofol and Morphine or Fentanyl. If your loved one is unstable and/o is showing signs of bleeding, sedation may be increased, in order to minimise further risk of bleeding and also to focus on haemodynamic stability first
- Your loved one will require monitoring using a Bedside Monitors and an Arterial Catheter(Arterial Line)
- You can expect your loved one to have frequent Chest X-rays and blood tests(Blood& Pathology tests in Intensive Care) especially arterial blood gases (ABGs), testing the effectiveness of the ventilation
- Infusion pumps are administering drugs to support your loved ones blood pressure and haemodynamic system, as well as intravenous fluids may be administered via a central venous catheter/ CVC(Central Venous Lines)
- Use of a Pulmonary Artery Catheters or a PICCO catheter to closely monitor cardiac function is not uncommon.
- An NG Tube (Nasogastric Tubes) is usually inserted into your loved ones stomach, in order to commence nutrition or to remove fluids
- Urine Output is usually measured hourly, after insertion of a Urinary Catheter
- An oxygen saturation probe attached to the your loved ones finger monitors the oxygen level in the blood continuously
- Monitoring of the drains chest drains(Under Water Seal Drain & Chest Tube) coming out of your loved ones chest, to drain any excess fluids of the surgery site and also to monitor any bleeding
- Abnormalities in heart rhythm usually require treatment
- Strict blood pressure control is achieved by medications infused via rate-controlled pumps. Fluid is also given intravenously at first to treat low blood pressure
- Body temperature is monitored. A blanket filled with warm air may be used to bring the body temperature back to normal
If you are visiting your loved one in the Intensive Care Unit at this stage you should expect to see many lines, tubes, and drains attached to your loved one.
What are the possible complications following CABG?
All surgery carries risks of complications. Possible complications following cardiac surgery include:
- Arrhythmia – irregular heart beat(i.e. Atrial Fibrillation/AF as the most common one, as well as Ventricular Tachycardia and Ventricular Fibrillation as less common ones)
- Excessive bleeding – may require returning to the operating theatre and a blood transfusion may be necessary
- Stroke – debris from the inner lining of the aorta (major blood vessel) can break off and lodge in the brain
- Infection – may occur in leg, arm or chest wound or in the chest
- Post-perfusion syndrome (pump-head), a transient neurocognitive impairment associated with cardiopulmonary bypass. Some research shows the incidence is initially decreased by off-pump coronary artery bypass, but with no difference beyond three months after surgery. A neurocognitive decline over time has been demonstrated in people with coronary artery disease regardless of treatment (OPCAB, conventional CABG or medical management). However, a 2009 research study suggests that longer term (over 5 years) cognitive decline is not caused by CABG but is rather a consequence of vascular disease
- Nonunion of the sternum; internal thoracic artery harvesting devascularizes the sternum increasing risk
- Myocardial infarction due to embolism, hypoperfusion, or graft failure.
- Late graft stenosis, particularly of saphenous vein grafts due to atherosclerosis causing recurrent angina or myocardial infarction
- Acute renal failure due to embolism or hypoperfusion
- Stroke, secondary to embolism or hypoperfusion
- Vasoplegic syndrome, secondary to cardiopulmonary bypass and hypothermia
- Grafts last 8 – 15 years, and then need to be replaced.
- Pneumothorax: An air collection around the lung that compresses the lung
- Hemothorax: Blood in the space around the lungs
- Pericardial Tamponade: Blood collection around the heart that compresses the heart and causes poor body and brain perfusion. Chest tubes are placed around the heart and lung to prevent this. If the chest tubes become clogged in the early post operative period when bleeding is ongoing this can lead to pericardial tamponade, pneumothorax or hemothorax.
- Pleural Effusion, fluid in the space around the lungs. This can lead to hypoxia which can slow recovery.
A member of the surgical team will discuss complications with your loved one prior to surgery. Any further questions you may have can be directed to the Intensive Care doctors and nurses.
What is the expected length of stay in the ICU ?
Most Patients will stay one or two days in the Intensive Care Unit following coronary artery bypass graft surgery and can be discharged home five to seven days later if things go well. However some Patients with complications will stay in the Intensive Care Unit for weeks or months.
What is life like after CABG surgery?
Following transfer from ICU to the ward your loved one will have the support of a multi disciplinary team to help get them back on their feet and ready for home. This team consists of doctors, nurses, physiotherapists, occupational therapists, dietitians, pharmacists, and social workers. The team gives advice on exercise guidelines and provides a program is for your loved one to return to usual activities for the weeks after discharge from hospital.
Your loved one is encouraged to attend a cardiac rehabilitation program that offers education sessions and supervised exercise programs. It also provides a valuable opportunity to meet with other people who have recently had heart surgery. Some hospitals also run a “Carer/Spouse Support Group” to address the needs of this group.
Some Patients find that they feel tired and have difficulty in concentrating after heart surgery. This is not unusual and should improve in approximately 4-8 weeks after surgery. Of course if you have any questions or issues, always discuss them with your doctor.
Internet Links
- http://www.heart.org/HEARTORG/ National Heart foundation USA
- National Heart Foundation – Australia
- National Heart Foundation – New Zealand
- British Heart Foundation
- Heart Beat Victoria
- MedicineNet – CABG
Any Questions?
Of course, if you have any questions or concerns, please discuss them with the ICU nurses and doctors.
All Intensive Care interventions and procedures carry a degree of potential risk even when performed by skilled and experienced staff. Please discuss these issues with the medical and nursing staff who are caring for your loved one.
The information contained on this page is general in nature and therefore cannot reflect individual Patient variation. It is meant as a back up to specific information which will be discussed with you by the Doctors and Nurses caring for your loved one. INTENSIVE CARE HOTLINE attests to the accuracy of the information contained here BUT takes no responsibility for how it may apply to an individual Patient. Please refer to the full disclaimer.
Related articles:
- Six weeks in Intensive Care after Cardiac Surgery and my mother isn’t getting any better…
- How long does a cardiac arrest patient stay in Intensive Care?
- How long can a breathing tube or an endotracheal tube can stay in?
- How long should a Patient be on a ventilator before having a Tracheostomy?
- How long is a Patient kept on a BIPAP machine in Intensive Care?
- What is an induced coma and why is my critically ill loved one in an induced coma?
- The 3 most dangerous mistakes that you are making but you are unaware of, if your loved one is a critically ill Patient in Intensive Care
- How to always achieve your goals whilst your loved one is critically ill in Intensive Care
- Why you must make up your own mind about your critically ill loved one’s situation in Intensive Care even if you’re not a doctor or a nurse!
- Follow this proven 5 step process on how to be in control and influential if your loved one is a long-term Patient in Intensive Care
- How to quickly take control and have real power and influence if your loved one is critically ill in Intensive Care
- Why does my loved one need a Tracheostomy in Intensive Care?
- Tracheostomy and weaning off the ventilator in Intensive Care, how long can it take?
- My sister has been in ICU for 21 weeks with Tracheostomy and still ventilated. What do we need to do?
- Severe lung failure and my aunty is not expected to survive…
- Be more selfish if your loved one is critically ill in Intensive Care
- 3 quick steps on how to position and prepare yourself well mentally, whilst your loved one is critically ill in Intensive Care
- How to get what you want whilst your loved one is critically ill in Intensive Care
- 5 steps to become a better negotiator if your loved one is critically ill in Intensive Care
- 5 Ways to have control, power and influence while your loved one is critically ill in Intensive Care
- How to make sure that your values and beliefs are known whilst your loved one is critically ill in Intensive Care
- How to make sure that “what you see is always what you get” whilst your loved one is critically ill in Intensive Care
- What the doctors and the nurses behaviour in Intensive Care is telling you about the culture in a unit
- How long does it take to wake up from a Traumatic brain injury or severe head injury
- How to take control if your loved one has a severe brain injury and is critically ill in Intensive Care
- Family Meetings in Intensive Care or the Elephant in the Room
- What you need to do if your loved one is dying in Intensive Care(part one)
- What you need to do if your loved one is dying in Intensive Care(part two)
- Intensive Care at its best?
- How INTENSIVECAREHOTLINE.COM Can Help You
- What you and your Family need to do if your critically ill loved one is very sick in Intensive Care and faces an uncertain future
- How long can somebody stay in Intensive Care?
- My Family can’t agree on what’s best for my sister in Intensive Care…Help!
- My husband is dying in Intensive Care, but we need more time…
- My mother sustained serious brain damage after a stroke and she now is in multi- organ failure


