Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM, where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have peace of mind, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
In the last blog I talked about
You can check out the last blog by clicking on the link here.
In this week’s blog I want to talk about
INTENSIVECAREHOTLINE.COM, why I do what I do. A story from behind the scenes!
Many families in Intensive Care that come to INTENSIVECAREHOTLINE.COM come to me and ask me why I do what I do and how I’ve come up with this idea of the INTENSIVECAREHOTLINE.COM support, advocacy, counselling and consulting website.
That’s only a fair question and I think it’s time that I share more about what I do and why I do it.
It’s quite simply that when I first went into nursing in 1996 I was full of enthusiasm and I wanted to help people in need.
That is still the case and I haven’t lost my enthusiasm to help people in need!
Much of it was driven by losing my uncle at the young age of 51 in Intensive Care after severe Cardiomyopathy in 1989.
Not that I knew then what me and my family were really dealing with, but it certainly shaped some views about the world I was living in.
When tragedy strikes everybody at first feels helpless and everybody is trying to clutch at straws.
Maybe me wanting to become a nurse was a sign of me trying to make sense of critical illness, death and everything else that goes along with it…
However, I sensed very quickly that I was in the right profession from the early days of my nursing career.
When I then first started in Intensive Care in 1999 I had no eyes for what’s happening “behind the scenes” in Intensive Care, I was just learning the clinical ropes and I was trying to get familiar in an overwhelming environment that was not short of challenges, including many difficult personalities.
I also realized that dealing with severe critical illness, dealing with death and dying and with stressed relatives of Patients wasn’t an easy task for a newbie and I once again felt very overwhelmed.
As time progressed and went on I felt more comfortable dealing with everything that was happening around me but I was nowhere near of having “embraced” the environment.
Fast forward after many more years in different environments and different countries in Intensive Care nursing, which included all major areas and specialities of Intensive Care including Trauma, Cardiac, Neuro, General, Medical, Surgical, Paediatrics and also Intensive Home Care nursing I also spent time working as a Nurse Unit Manager in Intensive Care for over 5 years.
Having managed two Intensive Care Unit was a lot of fun but also extremely challenging… I enjoyed every minute of it but I didn’t feel the need of wanting to do this for the rest of my life…
I gladly went back to the bedside, which is why I went into Intensive Care nursing in the first place.
But after I had spent more than a good decade in Intensive Care I could also see that “what you see is not always what you get” and I had learned enough to know and understand that the interests of an Intensive Care Unit and the interests of hospital management are not often the interests of a Patient and a family.
In fact, I sensed that there was often a real conflict of interest!
I had spent enough time in nurse/hospital/Intensive Care management as well as having worked with thousands of critically ill Patients and their families to understand on a deep level how vulnerable they felt.
And I understood on a deep level what questions they asked where Intensive Care Units are simply not telling families of critically ill Patients the truth.
I also understood what questions families in Intensive Care don’t ask, because they are worried to look stupid in front of others.
And I also understood what questions families in Intensive Care don’t even ask in the first place because they simply don’t know what they don’t know.
I learned that especially during incredibly challenging situations such as
Intensive Care Units and Intensive Care teams have huge interests way beyond your critically ill loved one’s diagnosis, prognosis, care and treatment and therefore if you and your family are not educated around those massively challenging and often heartbreaking situations, you often stand very little chance in getting what you want, need and deserve!
In the end, I wanted to create a safe environment for families in Intensive Care where any question can be asked and you will get an answer.
No hiding behind “hidden agendas” and no hiding behind “we are the experts here” which is what most Intensive Care teams do!
Related:
And here is another quick story from the real world in Intensive Care so that you really understand why I do what I do so that you get a feel for what’s often really happening in Intensive Care.
It’s also a story, why I eventually “pulled the trigger” so to speak, in making my vision a reality and have this support and resource website for families in Intensive Care.
I was working the Sunday night shift in a very busy ICU and I was looking after this 62 year old gentleman who fell off the roof of his house one day before on the Saturday.
The 62 year old man and his wife had just recently retired and they were looking forward to a much quieter life and they were looking forward to spend more time together after a busy working life.
When I came on to the night shift and after I received hand-over I realized things are not looking good and the 62 year old man had sustained severe intracranial bleeding and he also sustained multiple fractures around his ribs, HIP, arms and legs.
From what I’ve learned in ICU over the years, severe head and brain injuries tend to be some of the most challenging, unpredictable and also volatile injuries with sometimes a high probability of death.
This man’s situation wasn’t any different from many other severe head and brain injuries I looked after before. His CT of the brain was catastrophic with many areas showing bleeding into the brain, with a high chance of a non-survivable brain injury.
Furthermore, his intracranial pressures (=pressure in the brain) were very high, adding on further massive stress to the brain he didn’t need.
It was a very busy shift, trying to keep this 62 year old gentleman’s brain pressures at bay and we were doing whatever was necessary to keep him alive.
This was very much in line with what the family, mainly his wife and their two daughters wanted.
I didn’t have too much time on this shift to talk to the family as I was very busy, however what I realized was that this family spend all night at the bedside hoping and praying and trying to clutch at straws.
I knew that they weren’t prepared for everything that was happening, especially since their lives had changed literally overnight…
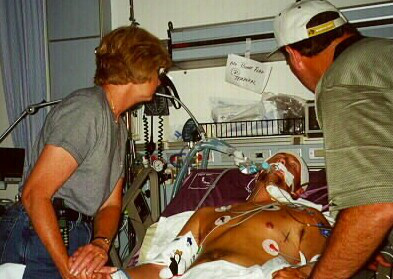
The 62 year old gentleman was very sick and his chances of survival were very slim…
I came back the next night only to find myself allocated again to the same Patient.
What came next left me absolutely speechless but also turned out to be a blessing in disguise.
After I received handover from my colleague from the day shift, I was told that by 10pm life support would be withdrawn and the 62 year old Patient was to be extubated (=removal of the breathing tube).
I felt like somebody kicked me in the guts.
I knew that this Patient was very sick with a very poor prognosis and I knew that his chances for survival were slim with such a massive bleed on his brain.
Apparently, the ICU team had a meeting with the family during the daytime and the family “was told” that life support would be withdrawn at 10pm tonight because it was “in the best interest” of the Patient.
The family wasn’t asked what they wanted for their husband and father.
The family wasn’t asked what they thought was “in the best interest” for their loved one!
One thing that I vividly remember was that I knew the family wasn’t emotionally ready for this. They knew and understood how sick their loved one was but they were nowhere emotionally ready to let go.
As my colleague finished handover the doctors passed by and did their ward round and the ICU consultant said to me “By 10pm you’ll be extubating this man”.
I looked him in the eye and said:
“If you want to extubate this man by 10pm you can do it yourself, because I’m not going to do it”.
He asked me if I was refusing to follow orders and I said to him.
“That’s exactly what I’m doing!”
I said to the ICU consultant that the family was nowhere near to be ready to let go and following his orders felt like following an order for an execution.
He looked at me and had nothing more to say.
Related:
I immediately went to the nurse in charge and reported to her about my serious concerns and also made very clear that I wasn’t going to follow those diabolical orders and that anything that was happening here was going against my moral and ethical values and beliefs!
I made very clear that if the family wasn’t involved in this decision making process that I would refuse to look after this Patient and either go home right here and then or they would have to reallocate me to another Patient.
On top of all of that, the family were waiting for their loved one’s brother to fly in from overseas.
When the doctors as well as the nurse in-charge realized that I was dead serious about what I was and what I wasn’t prepared to do, they actually started to listen and I said to them and the family that another family meeting needs to be held before any major decisions will be made.
The family was very appreciative that finally somebody was advocating for them.
Low and behold another family meeting was held that night with another ICU consultant who was willing to give the family more time to come to terms with things and who also made sure that all family members were there, including family members flying in from overseas.
Most ICU’s are pretty poor when it comes to end of life care. This one was a disaster and I have witnessed many poorly planned and poorly executed end of life situations. But this was extraordinarily poorly executed and I was determined to stop the way the ICU team went about it.
The Patient passed away about 48 hours after this debacle, but only after the family was given the opportunity to make an informed decision, have some peace of mind, a sense of control, power and influence.
After that I wrote a long email to nurse management in how disappointed I was to find myself in such a poorly planned end of life situation that caused a lot of stress for all parties involved.
But I also knew after this incident and after many other similar incidents that I witnessed over the years that it was time to act and start something where families in Intensive Care can have a voice, will be heard and also get an idea of what’s often really happening in Intensive Care!
Your friend
Patrik
How can you become the best advocate for your critically ill loved one, make informed decisions, get PEACE OF MIND, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care! Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below!
In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care!
In your FREE report you’ll also discover
-
- How to ask the doctors and the nurses the right questions
-
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
-
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
-
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
-
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
-
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
-
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s BLOG and I’ll see you again in another update next week!
Make sure you also check out our “YOUR QUESTIONS ANSWERED” section where I answer your questions or send me an email to [email protected] with your questions!
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling with me via Skype or over the phone and via email by clicking on the email and phone counselling tabs on the top of the website!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!



