Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM, where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from one of our readers and the question last week was
My Dad is in Intensive Care on BIPAP for COPD, should he be having a tracheostomy?
You can check out the answer to last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED“, I want to answer another question that we get quite frequently from our readers and the question this week is
What’s the average length of stay in Intensive Care after severe head or brain trauma(TBI)?
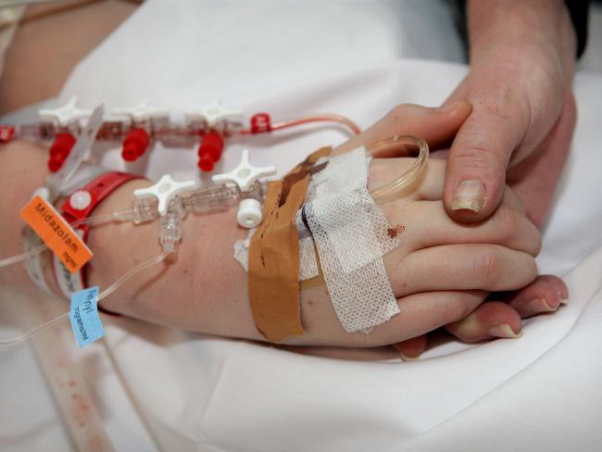
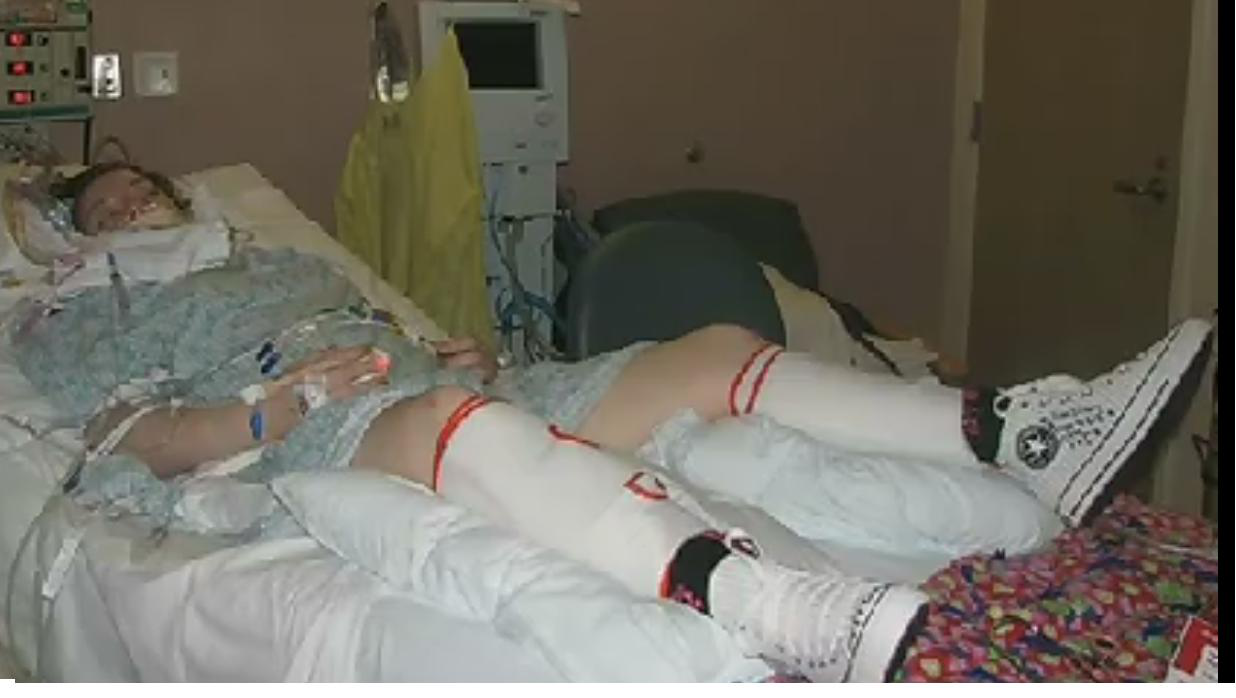
Quite a large number of people come to INTENSIVECAREHOTLINE.COM and they come to us because they have a loved one in Intensive Care who has a severe head or brain injury, also known as brain trauma or TBI.
If you want to know more about severe head or brain trauma(TBI) please check out our general section here
https://intensivecarehotline.com/clinical-pictures/traumatic-brain-injury-tbi/
Most Patients ending up in Intensive Care with a severe head or brain injury or brain trauma usually have events leading up to it like a Motor vehicle or motorbike accidents, they fall off a roof, they might be in a fight etc…
For anyone with a severe head or brain injury the first life savings steps are to be admitted to Intensive Care after they have been through the emergency room and/or the operating theatre.
Part of the first 24 hours in hospital/ Intensive Care should also include a CT of the brain to determine the severity of the brain injury or brain trauma.
Head and brain injuries come in different shapes and sizes and once it’s been confirmed that a severe head or brain trauma has been sustained head or brain surgery might be one of the next steps to remove any significant bleeds if possible, sometimes to remove parts of the skull (=Craniectomy) and sometimes to insert an EVD (=Extraventricular drainage), a Codman’s or an ICP monitor.
In any case, the first few hours and the first few days after a significant brain trauma or brain injury include to maximise the chances of survival for your critically ill loved one and that can sometimes be very challenging especially when ICP’s (=Intracranial brain pressures) are high and elevated. ICP’s are basically the pressure in the brain.
If the pressure in the brain is too high and goes >20 mmHg there is the risk of significant and also irreversible brain damage.
In order to achieve an ICP(=Intracranial brain pressure) <20 mmHg usually a minimum of 60 mmHg of CPP(=Cranial Perfusion pressure) needs to be achieved in order to achieve sufficient oxygen supply to the brain.
The higher the ICP the lower the CPP and therefore the increased risk of insufficient oxygen perfusion to the brain could cause irreversible brain damage.
You can find more information about ICP’s here
https://intensivecarehotline.com/intracranial-pressure-monitoring/
Mechanisms to manage high ICP’s are to drain CSF(=brain and spinal fluid), give hypertonic Saline, give Mannitol, keep CO2(Carbondioxide) down by hyperventilating, by using strong sedation and strong pain relief as well as using specific sedatives for TBI’s such as Thiopentone.
Once of all of these therapies have been maximised and hopefully ICP’s and CPP’s can be controlled and managed then it will very often be a “waiting game”.
What do I mean by that?
Critically ill Patients with severe and significant head or brain injuries are some of the most difficult Patients to look after especially when they are not doing well and ICP’s and CPP’s are difficult to control.
Any time ICP’s are too high for prolonged periods and in theory for more than 3 minutes, there is the risk for irreversible brain damage.
Because of such high risk for irreversible brain damage, Intensive Care teams tend to be very negative from the start and they are therefore often trying to position your critically ill loved one’s diagnosis, their prognosis, as well as their care and their treatment in a negative light and they often hint towards “withdrawing treatment” as “in the best interest” for your critically ill loved one.
With the negativity of the Intensive Care team as well as with the positioning of the Intensive Care team very early on that a “withdrawal of treatment” or a “withdrawal of life support” might be “in the best interest” for your critically ill loved one they are also implying that they don’t want to exceed a certain length of stay in Intensive Care.
Whenever the Intensive Care team says that they think that a “withdrawal of treatment” or a “withdrawal of life support” is “in the best interest” for your critically ill loved one they are in essence saying that your loved one’s stay in Intensive Care is not welcome for prolonged periods.
Related:
You see, there are so many moving parts in Intensive Care, especially the parts “BEHIND THE SCENES” that only insiders like myself know about…
You and your family wouldn’t have any clue about what a “withdrawal of treatment” and a “withdrawal of life support” for your critically ill loved one really means.
From my experience after nearly 20 years Intensive Care nursing in three different countries, where I literally worked with thousands of critically ill Patients and their families and where I also worked as a Nurse Unit Manage for more than 5 years and also through my 1:1 phone/Skype and email counselling and consulting for families in Intensive Care, the best outcomes for severe head and brain injuries are usually achieved when time, nurturing and world class care are being provided in a positive environment.
This in and of itself leads us much closer to our original question that I set out to answer
What’s the average length of stay in Intensive Care after severe head or brain trauma(TBI)?
The answer is that it really depends.
If you are like 99% of the families of critically ill Patients in Intensive Care who make no informed decisions, have no peace of mind, no control, no power and no influence you will most likely don’t question or second guess when the Intensive Care team is telling that your critically ill loved one is having a poor prognosis and that it’s “in the best interest” for your critically ill loved one to “withdraw treatment” or “withdraw life support”.
Other statements that the Intensive Care team often uses to cement and support their positioning when it comes to “withdrawal of treatment” and “withdrawal of life support” after severe head or brain injuries/TBI’s include statements like, your critically ill loved one wouldn’t want to be a “vegetable” or “your critically ill loved one wouldn’t have any quality of life”.
If you and your family are unprepared for any of the Intensive Care team’s positioning of your critically ill loved one’s diagnosis and their prognosis, as well as their care and their treatment then the length of stay FOR YOUR CRITICALLY ILL LOVED ONE will be short and the Intensive Care team will be in control, period!
If you are like 99% of the families of critically ill Patients in Intensive Care who make no informed decisions, have no peace of mind, no control, no power and no influence you, your family and your critically ill loved one will stay at the mercy of the Intensive Care team and you will most likely feel intimidated by their “perceived power” and their “perceived authority”.
The best outcomes for severe and significant head or brain injuries and the maximisation of survival usually comes after sometimes many weeks if not many months in Intensive Care.
I remember many years back when I worked in my first nursing job in Intensive Care, we had a young Patient who fell off a roof and he had a significant head and brain injury.
He was in Intensive Care for nearly six months and it took a long time for him to recover. He was extremely sick and he went through many many trials and tribulations to leave Intensive Care alive.
He had prolonged periods with high ICP’s and eventually he went into kidney failure and he had to be dialysed.
But the bottom line was that nobody was ever given up hope for this young man and he eventually pulled through and got out of Intensive Care alive.
He also visited the Intensive Care unit about 6 months later to show everybody that he’s alive and well and he wanted to show his gratitude to the people who looked after him. At the time he was back in a job already and he was going to get married too!
Therefore, the answer to
What’s the average length of stay in Intensive Care after severe head or brain trauma(TBI)?
Is very much dependent not only on the culture of the Intensive Care Unit but also on your mindset and also how much you buy into the negativity of the Intensive Care team.
It’ll also come down to how prepared you are to fight for your critically ill loved one and it’ll also depend on if you are doing your own research or if you engage a consultant like myself!
Again, if you and your family are like 99% of the families of critically ill Patients in Intensive Care you’ll make no informed decisions, you have no peace of mind, no control, no power and no influence and you are probably intimidated by the “perceived power” and the “perceived influence” of the Intensive Care team.
If you are in the tiny little 1% bracket of families in Intensive Care you’ll fight, you do your own research and you’ll seek out advice like in my 1:1 counselling and consulting service and you simply won’t take “no” for an answer.
Therefore the answer to
What’s the average length of stay in Intensive Care after severe head or brain trauma(TBI)?
Is an answer that you have more control over than you think you have, if you do your own research, if you advocate for your critically ill loved one, if you’re not intimidated by the Intensive Care team and if you keep looking in how you can start managing the dynamics with the Intensive Care team and not the other way around.
Intensive Care teams are the master at managing the dynamics with families in Intensive Care and they know what to say, they know when to say it, they know how to say it and they know what not to say to stay in control of the meaning and to stay in control of the outcomes that they want.
The outcomes that the Intensive Care team wants is most of the time not aligned with the outcomes that you want.
The outcomes the Intensive Care team wants is dependent on the “hidden agenda” and on the things happening “BEHIND THE SCENES” in Intensive Care.
The outcomes you and your family want is to maximise the chances for survival for your critically ill loved one.
Also, what does it mean for you and your family if your loved one is critically ill in Intensive Care with a severe head and brain injury/TBI?
Have you given it some meaning? I hope you have, because the Intensive Care team will give it their meaning and you probably don’t like it…
Related article/video:
“Waking up” or not “waking up”?
The next often “life or death” issue that families in Intensive Care are facing after their loved one sustained a severe head or brain injury/TBI is that once your loved one is coming out of the induced coma that they may not be “waking up” in a time frame that is convenient for the Intensive Care team.
What do I mean by that?
Well “waking up” after an induced coma can sometimes be prolonged and “waking up” after a severe head or brain injury can be even more prolonged and if the Intensive Care team thinks that your critically ill loved one is “waking up” in a time frame that’s convenient for them, they again might tell you that a “withdrawal of treatment” or a “withdrawal of life support” is “in the best interest for your critically ill loved one.
At the end of the day, if the Intensive Care team is not prepared to invest the time, the money, the physical as well as the emotional resources needed to get your critically ill loved one out of Intensive Care alive, the negativity will always be their fallback position.
There is just too much at stake for the Intensive Care team such as their financial budget, their bed management issues, their staffing and other resources, their medical research interests as well as the politics, the hierarchies, the intrigue, the psychology and the list goes on.
Therefore if the Intensive Care team has been negative from the start, which is very likely and if they continue to be negative because your critically ill loved one is not “waking up” you’d better be prepared and challenge the Intensive Care team.
Recommended:
Before I close this subject for today, I also want to quickly give you two examples from my own inner circle, where my cousin’s husband many years ago endured a severe head and brain injury and he spent many weeks and many months in Intensive Care and rehabilitation and yet he is ever so grateful to be alive!
Another friend of mine that I used to go to school with also sustained a severe head and brain trauma and he was in ICU and rehabilitation for many many months. Again if he didn’t get good care, treatment, positivity and nurturing he wouldn’t be alive today.
Both are prime examples that the length of stay in Intensive Care matters and not giving up and not taking “no” for an answer matter too!
The question really is will you and your family have the Intensive Care team dictate to you how long your loved one is to stay in Intensive Care after a severe traumatic brain injury or will you be calling the shots?
Your friend
Patrik Hutzel
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!