Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM, where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question last week was
What are reasons for not being able to come off the ventilator/respirator?
You can check out the answer to last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED“, I want to answer another question from one of our readers and the question this week is
My sister is in Intensive Care after a car accident with multiple fractures. The doctors want us to “pull the plug”, we want to keep going, what are our rights?
This question from Barbara is an excerpt from an email counselling and consulting session with me.
Barbara writes
Hi Patrik,
my sister is in intensive in the shock trauma ICU unit xxxxxxxxxxx Hospital. She was in a car accident a few weeks back and she is very overweight.
After four weeks of extensive treatment, the Intensive Care doctors were painting more and more of a doom and gloom picture of her being on a ventilator and needing to be in a nursing home for the rest of her life.
She has a broken hip which they operated on, her neck is in a brace she has a crushed vertebra with a rod which was successfully inserted in her back.
Thankfully she sustained no head or brain injuries, therefore she is now slowly “waking up” and she seems to be getting more and more alert and she seems to have a better understanding of her surroundings and of what’s going on.
She has now gone from the ventilator with a breathing tube to a trachea on a ventilator only about 10 days ago. She is being suctioned regularly because she is not able to cough, speak, eat or drink.
They have now started to try and wean her off the ventilator in the last couple of days and she barely manages two hours off the ventilator during the day.
She is 73 and that’s not very old from my perspective. The Head Doctor wants us to pull the plug and let her die if she cannot breathe. He says that my sister wouldn’t have any quality of live if she stays on the ventilator for the rest of her life.
We want her to live and at least give her the best chances to live, what are our rights and what are our options? Please help!
Many thanks
Barbara
Here is my answer,
Hi Barbara,
thank you for your question and thank you for using my 1:1 email counselling and consulting services.
I’m very glad to hear that your sister has a great advocate by her side which is yourself and also the rest of your family!
It’s good that you and your family want your sister to live and by everything you are describing, I think she has a very good chance to live!
Four weeks in Intensive Care after multiple trauma (Polytrauma) is nothing unusual.
I often see part of my role to give people perspective when they have a loved one critically ill in Intensive Care.
Again, four weeks after multiple trauma with multiple surgeries is nothing in the bigger scheme of things even though it must feel like an eternity and a never ending nightmare for your sister, for yourself and for the rest of your family.
Again, going from ventilation with a breathing tube (Endotracheal tube) to a tracheostomy on the ventilator is nothing unusual after Multiple trauma (Polytrauma).
I have seen this scenario play out over and over again.
Now, the doctors are implying that your sister will need ventilation for the rest of her life and they haven’t even started to try and wean her off the ventilator properly.
Weaning your sister off the ventilator can take time and given that you have described that she barely manages two hours off the ventilator for the last two days, they haven’t even scratched the surface.
They need to as a starting point increase the time she can tolerate off the ventilator gradually and slowly.
Weaning a critically ill Patient off the ventilator with tracheostomy can sometimes be a marathon and not a sprint.
Taking a negative spin and painting the typical “doom and gloom” picture that ICU’s often paint doesn’t help.
That’s why it’s so important that you and your family remain strong, make informed decisions, have peace of mind, control, power and influence during this crucial time in your sister’s and in your family’s life!
Again, the first few weeks after the accident the focus was to get the multiple fractures in order your sister sustained.
After that has been done, the next step is to try and wean her off the ventilator and then hopefully the tracheostomy can be removed next.
It’s almost the same old story over and over again, Intensive Care Units are getting better and better at saving lives and yet, once they have done that and gotten your sister through all this treatment to get her fractures operated on and give her a tracheostomy, then they want you to agree to “pull the plug”.
If you have followed my blog and my “your questions answered” episodes you would know by now that Intensive Care doctors wanting to “pull the plug” is rarely the right thing to do.
I have written extensively about what’s a “real” and what’s a “perceived” end of life situation and you can check it out here.
The next step for your sister is to get her out of bed and mobilized.
That’ll strengthen her body and also her breathing. Getting Patients out of bed as early as possible is very important when it comes to weaning her off the ventilator/respirator.
It’s also stimulating for your sister and she’ll need stimulation after four weeks in Intensive Care whilst being in an induced coma most of the time.
She will also need Physical therapy or Physiotherapy as soon as possible to get her back to moving if she can.
Physical Therapy or Physiotherapy will also help with strengthening her breathing muscles to get her off the ventilator.
That in and of itself sounds much more appealing compared to the negativity from the Intensive Care team and it sounds way more appealing compared to the Doctors asking you to agree to “pulling the plug”!
Many Intensive Care teams are simply not prepared to work through the challenges of a prolonged stay in Intensive Care when Patients are being ventilated with tracheostomy.
Related article/video:
But it’s not only the clinical challenges that are an issue, it’s also that a long-term stay in Intensive Care may not be financially viable for the Intensive Care team.
Furthermore, by weaning your sister off the ventilator she may be blocking a bed that the ICU could use for another often more financially viable Patient. After all ICU beds are precious, scarce, expensive and “in-demand”!
Moreover, Intensive Care Units are also doing a lot of medical research and if your sister can’t be enrolled in a medical research study, again the interest might be low to help her leaving Intensive Care alive.
And most of all, besides financial and other resources such as staff and equipment being needed, the Intensive Care team simply doesn’t want to make the emotional investment to get your sister out of Intensive Care alive and give her the best possible chance to get off the ventilator.
It’s all part of the Intensive Care team’s “hidden agenda” that you and your family know nothing about!
Related:
Therefore, even if I sound like a broken record, four weeks in Intensive Care after multiple trauma and only having the tracheostomy for 10 days now is not a very long time and you and your family know that!
The Intensive Care team knows it too but they simply don’t want to continue on the path to improvement because it seems too much effort and “pulling the plug” maybe a much “easier” option.
Again, from my perspective and from my experience you are only at the start of what maybe a long road of recovery and you’d be surprised what can happen if you stay positive, patient and persistent!
“Pulling the plug” is not an option from all the information that you’ve given me and if they are trying to wean your sister off the ventilator there can’t be many other forms of life support, therefore as a matter of fact no matter how hard the Intensive Care team is trying, it’ll be hard for them to “pull the plug” if the only major life support your sister is on is the mechanical ventilation!
Also, in order for the Intensive Care team or the doctors to want you to “pull the plug” or to “withdraw treatment” they need to follow certain protocols, policies and guidelines and even the law.
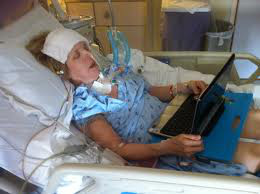
“Withdrawing treatment” or “pulling the plug” Is not as easy as it sounds even though the Intensive Care team is trying to make it look easy.
Recommended:
And it’s good to see that you are trying to seek help, advice and advocacy.
Rather than talking about “pulling the plug” or “withdrawing treatment” or “limiting life support”, we should be looking at solving the problem so that your sister can leave Intensive Care alive so that she can have the best possible quality of life!
The best way to go about is to wean her off the ventilator, get her out of bed and stick to a daily regime so that your sister can get back to “normality” as quick as possible.
If your sister can tolerate it she should start with one or two hours off the ventilator every day and then gradually increase her time off the ventilator with two hours on and two hours off the ventilator. The next step is to then get her off the ventilator throughout the whole day and then ventilation overnight.
Then at some point she can hopefully stay off the ventilator for >24 hours.
None of that may happen overnight and can sometimes take many days, many weeks and sometimes many months.
You’ve already figured that the alternative with “pulling the plug” is not an option!
Again, as I mentioned before, mobilisation out of the bed is part of weaning off the ventilator too and it needs to happen rather sooner than later.
Good pain control is essential when mobilising, especially with your sister’s injuries!
Don’t be discouraged if there are setbacks, they can happen.
For example, I have been working with another client over the last few weeks and the client’s family member was in ICU for about 8 weeks and initially couldn’t be weaned off the ventilator and the tracheostomy.
The client’s family member only lasted around 10 minutes off the ventilator initially and then gradually increased his time off the ventilator until he could finally get weaned off the ventilator and had the tracheostomy removed.
Also, please keep in mind that if your sister can’t be weaned off the ventilator or if you’d rather have your sister being weaned off the ventilator at home, take a look at INTENSIVE CARE AT HOME
INTENSIVE CARE AT HOME is a fully accredited Intensive Home Care service provider and we can do what Intensive Care Units or LTAC’s can do as well, just in a much more Patient and family friendly environment.
Therefore your sister can improve her quality of life at home as well rather than in an inhibiting, negative, sterile and depressing hospital and/or Intensive Care environment.
I find it highly inappropriate if the Doctor keeps talking about quality of life without having asked you or your sister what quality of life is acceptable for her. Quality of life is a very subjective experience and it doesn’t really matter what the doctor thinks about it.
All that matters is what you, your family and your sister think and are happy with, those are the most important things.
Your sister has come thus far, there is no reason why she can’t go further.
Your friend
Patrik Hutzel
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!



