What is an Intra-Aortic Balloon Pump(IABP)?
The Intra-aortic balloon pump (IABP) is a mechanical device that increases oxygen perfusion in the heart and the heart muscles, while at the same time increasing cardiac output(blood flow). Increasing cardiac output increases coronary blood flow and therefore myocardial oxygen delivery(oxygen delivery to the heart). It consists of a balloon that sits in the aorta(main artery and biggest vessel in the body, sitting right underneath the heart). That is, it actively deflates when the ventricles of the heart contract and eject blood, increasing forward blood flow by reducing the resistance after the heart(afterload). It actively inflates when the ventricles of the heart relax(diastole) and refill with blood, increasing blood flow to the coronary arteries(arteries supplying the heart with oxygen). These actions combine to decrease oxygen demand for the heart and increase oxygen supply to the heart.
A computer-controlled mechanism inflates the balloon with helium from a cylinder during diastole, usually linked to either an electrocardiogram (ECG) or a pressure transducer at the distal tip of the catheter; some IABPs allow asynchronous counter-pulsation at a set rate, though this setting is rarely used. Helium is used because its low viscosity allows it to travel quickly through the long connecting tubes, and has a lower risk than air of causing an embolism should the balloon rupture.
How Does It Work?
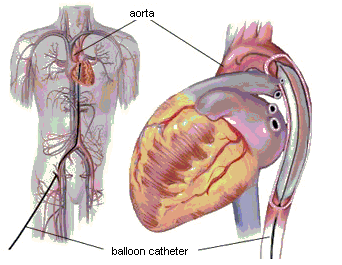
The IABP is connected to a long catheter. The balloon at the end of the catheter is sitting right in front of the heart in the aorta. The catheter is inserted via the left or right groin(femoral artery). The IABP’s pumping rhythm is synchronised with your loved ones heart rhythm and the helium gas is inflated and deflated in sync with the heart beats.
What is it used for?
The following situations may benefit from this device.[2][3][4]
- Cardiogenic shock when used alone as treatment for Heart Attack(Acute Myocardial Infarction)
- Reversible intracardial mechanical defects complicating a heart attack, i.e. acute mitral valve deficiencies
- Unstable angina pectoris benefits from IABP
- Post cardiothoracic surgery(Coronary Artery Bypass Graft (CABG))
- Before heart surgery, use is suggested for high-risk Patients such as those with unstable angina with stenosis greater than 70% of main coronary artery, in ventricular dysfunction with an ejection fraction less than 35%.
- Percutaneous coronary angioplasty
- Thrombolytic therapy after Heart Attack(Acute Myocardial Infarction)
- Cardiac Arrest
How Long Will It Be Used For?
The IABP is a short term and temporary solution to support a severely weak heart after Cardiac Surgery(Coronary Artery Bypass Graft (CABG)), after a Heart Attack(Acute Myocardial Infarction) or after a Cardiac Arrest has been sustained. It will only be used for a few days, up to one week in rare instances. The longer the IABP stays in place the higher the risk for infection.

Are There Any Complications?
Since the device is placed in the femoral artery(groin) and aorta it could cause ischemia(tissue death due to lack of oxygen), and compartment syndrome. The leg is at highest risk of becoming ischemic(tissue death due to lack of oxygen), if the femoral artery it is supplied by, becomes obstructed. Placing the balloon too low in the aorta may induce occlusion of the renal artery and subsequent renal/kidney failure. Other possible complications are cerebral embolism during insertion, infection, dissection of the aorta, perforation of the artery and bleeding(hemorrhage) in the mediastinum. Mechanical failure of the balloon itself is also a risk which entails vascular surgery to remove under that circumstance. After balloon removal there is also a risk of ’embolic shower’ from micro clots that have formed on the surface of the balloon, and can lead to peripheral thrombosis and lack of oxygen supply to the heart.
Any Questions?
Of course, if you have any questions or concerns, please discuss them with the ICU nurses and doctors.
All Intensive Care interventions and procedures carry a degree of potential risk even when performed by skilled and experienced staff. Please discuss these issues with the medical and nursing staff who are caring for your loved one.
The information contained on this page is general in nature and therefore cannot reflect individual Patient variation. It is meant as a guideline to specific information which will be discussed with you by the Doctors and Nurses caring for your loved one. INTENSIVE CARE HOTLINE attests to the accuracy of the information contained here BUT takes no responsibility for how it may apply to an individual Patient. Please refer to the full disclaimer.
How can you have PEACE OF MIND, control, power and influence whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below! In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care! Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below!
In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care!
In your FREE reports you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 “killer” tips& strategies helping you to get on the right path to PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘BEHIND THE SCENES’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care(it’s not what you think)
Make sure you also check out our “blog” section for tips& strategies and also check out our “your questions answered” section where we answer your questions or send me an email to [email protected] with your questions!
Sincerely, your Friend
Patrik Hutzel
Related articles:


