Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM , where we instantly improve the lives of Families of critically ill Patients in Intensive Care, so that you can have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from one of our readers and the question last week was
You can check out last week’s question here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer another question that we get asked quite frequently and the question this week is
“HOW LONG can a critically ill Patient stay on ECMO?”
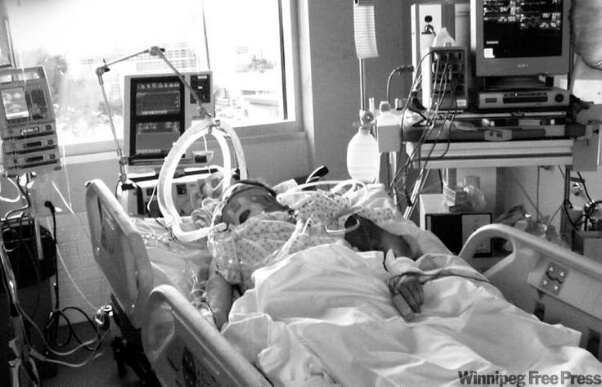
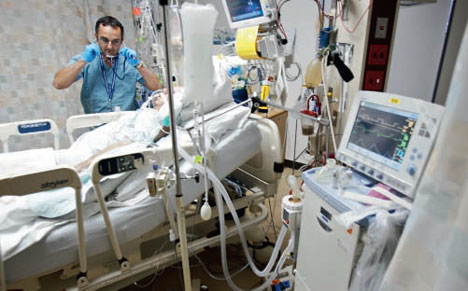
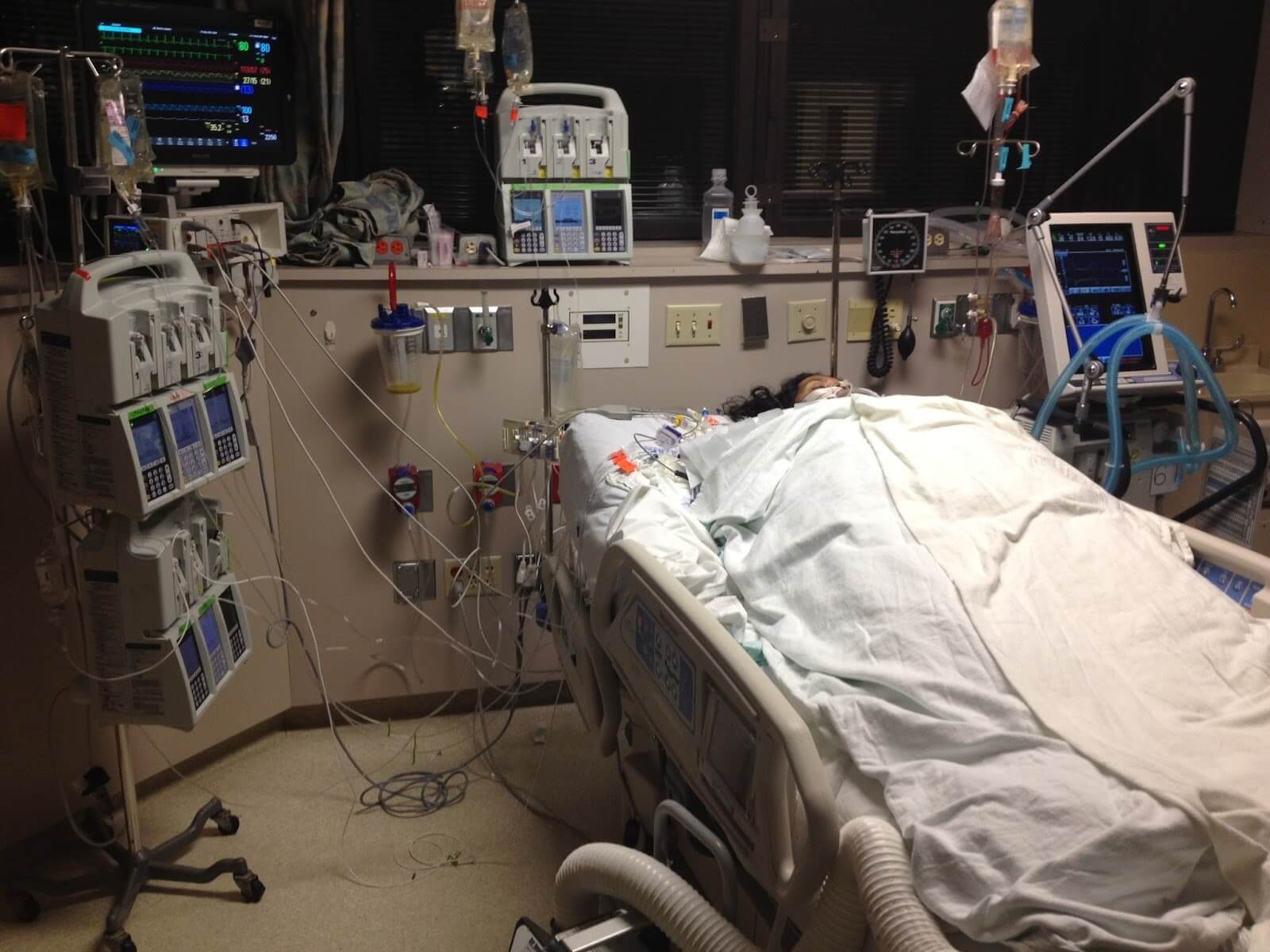
Now if your loved one is critically ill in Intensive Care and requires ECMO(Extracorporeal membrane oxygenation) for either heart failure(heart attack, Cardiomyopathy, cardiac arrest, cardiogenic shock or as a bridge to LVAD and/or heart transplant) or lung failure(ARDS, Cystic fibrosis and as a bridge to lung transplant) you might be wondering how long your critically ill loved one can stay on the ECMO machine.
It’s a fair, reasonable and very important question to ask and many of our readers want to know about it.
First of all, your critically ill loved one has either heart failure or lung failure and therefore requires the ECMO therapy.
ECMO for heart failure is also being referred to as VA-(Veno- Arterial) ECMO and ECMO for lung failure is being referred to as VV(Veno- venous) ECMO.
The difference is simply that the big cannulas being used for ECMO are either going from the vein to the artery in ECMO for heart failure and in ECMO for lung failure, the big cannulas for blood extraction and blood return are from vein to vein.
ECMO is a relatively new therapy in Intensive Care
In any case, you and your family need to keep in mind at all times that ECMO is a relatively new therapy in the bigger scheme of things and has only been around for the last 10- 15 years.
It’s therefore a relatively new therapy.
Therefore you could expect that there is still a lot of testing and “trial and error” going on, given that it’s such a new therapy in the Intensive Care/ Critical Care world.
If your critically ill loved one is on ECMO for either heart failure or lung failure, the purpose for both ECMO variations is generally speaking to give the sick organ(heart or lung) a rest and let them recover.
In either, VA- ECMO(for heart failure) or VV- ECMO(for lung failure) the purpose of either is to let the heart or the lungs rest and let the ECMO machine take over the function of either the heart or the lung.
That’s being achieved by having the gas exchange taking place in the ECMO machine. Oxygen(O2) is being delivered into the blood via the ECMO machine and carbon dioxide(CO2) is being removed via the ECMO machine.
In either VA- ECMO for heart failure or VV- ECMO for lung failure your critically ill loved one is most likely being ventilated and in an induced coma.
Sometimes being awake on ECMO is a rare option
There is the option, especially for critically ill Patients in heart failure and therefore on VA- ECMO to be breathing spontaneously and without the ventilator, therefore being awake and not in an induced coma.
This can be the preferred option, especially given that ventilation and induced coma come with massive side effects and high risks.
However being awake and on ECMO can also be challenging, as Patients are awake and fully aware of their often difficult situation.
This can have other psychological challenges as Patients may get depressed and/or panicky about their critical situation.
Withdrawal of treatment can be morally and ethically challenging in ECMO Patients
It could get particularly challenging(morally, ethically and clinically) if treatment would be withdrawn on an awake Patient.
If your critically ill loved one requires ECMO for lung failure(VV- ECMO) it is less likely that your critically ill loved one is being awake and off the ventilator. Whilst this may be possible in some critically ill Patients, it is less likely to occur on VV- ECMO for lung failure.
It’s also more likely that f if your critically ill loved one requires VV- ECMO for lung failure that they may end up with or already have a Tracheostomy.
Tracheostomy may be an option
A Tracheostomy may be required if a prolonged weaning off the ventilator is expected. In a critically ill Patient on VV- ECMO for lung failure a prolonged weaning off the ventilator after ECMO has been discontinued is often likely and therefore a Tracheostomy necessary.
Related Article:
How long should a Patient be on a ventilator before having a Tracheostomy?
In any case, a Tracheostomy is often the better option for your critically ill loved one if prolonged ventilation is required, as the ventilation therapy can be easier tolerated with a Tracheostomy.
Having said that if a Tracheostomy is required for either VV-ECMO(for lung failure) or VA- ECMO(for heart failure) the procedure for a Tracheostomy might get delayed as both variations of ECMO require high doses of Heparin(a blood thinning medication) and therefore increase the risk for severe bleeding if a Tracheostomy was to be performed.
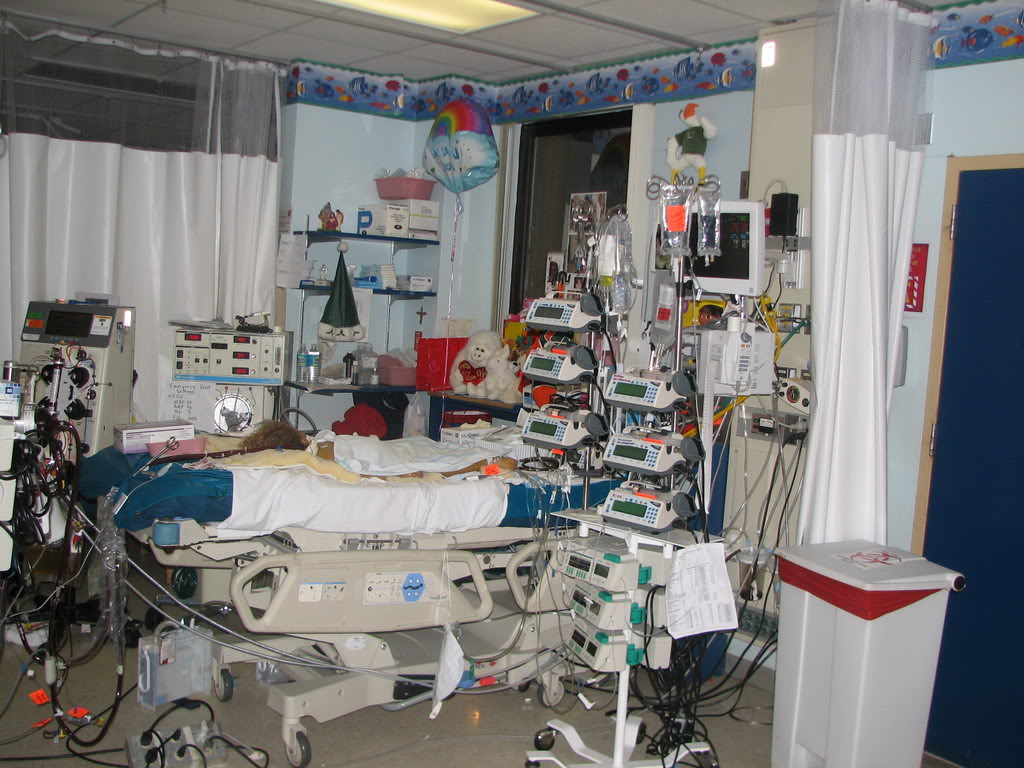
Finally, in either VV-ECMO(for lung failure) or VA- ECMO(for heart failure) the length of time a critically ill Patient can stay on ECMO depends on the severity of the heart or lung failure and can also depend on other factors such as age, pre- medical history or the co-morbidities your critically ill loved one may have.
2-3 weeks on ECMO is generally speaking the maximum time
As a rule of thumb, 2-3 weeks is probably the longest I have seen for a critically ill Patient to be on either VV-ECMO(for lung failure) or VA- ECMO(for heart failure).
The risks being on either VV-ECMO(for lung failure) or VA- ECMO(for heart failure) tend to be pretty significant, with large cannulas being inserted into the body and other risks such as ventilation, sedation, induced coma, inotropes, immobilisation, anticoagulation therapy(i.e. Heparin for blood thinning) often put a strict time limit on the high- risk therapy.
If two to three weeks don’t give the heart or the lungs enough time to recover from their initial disease or weakness, in heart failure, an insertion of an LVAD would be the logical next step or a heart transplant.
If your critically ill loved one suffers from lung failure and requires prolonged and high risk VV- ECMO therapy and can’t be weaned off the machine, a lung transplant might be the next possible step.
Again, in either VV-ECMO(for lung failure) or VA- ECMO(for heart failure) your critically ill loved one would have to undergo a weaning process so that either the heart or the lung can recover and take over their normal or physiological function and then the ECMO can be gradually weaned and then removed.
In VV-ECMO(for lung failure) the weaning process would go hand in hand with chest x-rays and with checking of arterial blood gases to check and monitor the adequacy of the gas exchange in the lungs.
In VA- ECMO(for heart failure) the weaning process goes hand in hand with more formal weaning studies such as an Echoecardiography of the heart and/or TOE.
A reduction of Inotropes(medication for low blood pressure management) would be necessary as well.
You should also be having some strategies in place if the Intensive Care team suggests to withdraw treatment and to withdraw the ECMO therapy on your critically ill loved one, as you need to be prepared for any challenges in Intensive Care.
Sometimes the Intensive Care team suggests the withdrawal of treatment or the withdrawal of life support as being “in the best interest” of your critically ill loved one.
The reality and the fact of the matter is that if you are not prepared for those situations you will have no PEACE OF MIND, no control, no power and no influence.
If you don’t understand what’s happening in Intensive Care “BEHIND THE SCENES” and if you don’t understand how the Intensive Care team is making decisions that often go way beyond your critically ill loved one’s diagnosis and prognosis, you will have a hard time to have PEACE OF MIND, control, power and influence!
Related articles:
Recommended resources:
You should in any case continue doing your own research whilst your loved one is critically ill in Intensive Care.
You should also not take anything the Intensive Care team is telling you for “FACE VALUE”!
You should continue to look for strategies how you can proactively manage the Intensive Care team that when it comes to difficult and challenging situations that you have bargaining power, PEACE OF MIND, control, power and influence!
How do you do that and how can you have PEACE OF MIND, control, power and influence whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below! In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care! Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 “killer” tips& strategies helping you to get on the right path to PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care(it’s not what you think)
Thank you for tuning into this week’s “YOUR QUESTIONS ANSWERED” and I’ll see you again in another update next week! Make sure you also check out our BLOG section for more tips and strategies or send me an email to [email protected] with your questions!
Also check out our Products section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 consulting!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!
Related Articles
- 6 phrases you should never say when your loved one is critically ill in Intensive Care
- How to REPROGRAM YOUR MIND if your loved one is critically ill in Intensive Care
- How to play a “HIGH STAKES GAME” that only the Intensive Care team knows HOW TO WIN!
- Family overjoyed as top court rules doctors must seek consent before taking a patient off life support
- How to make sure that your values and beliefs are known whilst your loved one is critically ill in Intensive Care
- CAN YOU GO HOME ON A VENTILATOR?
- DISRUPT before you are being DISRUPTED, whilst your loved one is critically ill in Intensive Care!
- How MEDICAL RESEARCH DOMINATES your critically ill loved one’s diagnosis and prognosis, as well as the CARE and TREATMENT your loved one IS RECEIVING or NOT RECEIVING
- 5 things NOBODY HAS EVER TOLD YOU about Intensive Care!
- WHAT WOULD YOU DO if you knew that you COULD NOT FAIL, whilst your loved one is critically ill in Intensive Care?