Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM, where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question last week was
You can check out the answer to last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer another question from one of our readers and the question this week is
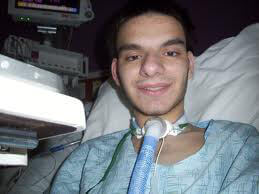
My 59 year old Dad is in ICU after cardiac arrest! He had to be resuscitated for 18 minutes, will he have brain damage?
This question from Sarah has been part of an email counselling and consulting session with me!
Sarah writes,
Hi Patrik,
my father has been in intensive care for just over a week. He had a cardiac arrest for 18 mins while the doctors and the nurses were trying to resuscitate him.
They did two CT scans, one for his brain and one on his chest hours after the doctors revived him and the same again two days ago for follow up.
Both CT’s are mainly clear but show a black shadow on the left brain which indicates an old stroke a few weeks before the cardiac arrest. The CT on his chest also show a pleural effusion that they have drained with a chest drain.
They also started him on cooling therapy for 72 hours after the cardiac arrest.
Apart from that no other damage to the brain according to the doctors. He’s diabetic and has high blood pressure, sleep apnea, kidney problems etc. He’s 59 and he is still sedated. We are just worried he may be brain damaged. But he opens his eyes and mouth then falls back asleep. Please help!
Sarah
Hi Sarah,
Thank you for sending this question through and thank you for signing up for my 1:1 email counselling and consulting!
I’m very sorry to hear what you and your family are currently experiencing with your Dad being in ICU after his cardiac arrest!
Let’s look at the positives first!
There is no apparent brain damage from the cardiac arrest!
That means that the resuscitation of 18 minutes after/during the cardiac arrest must have been successful and effective.
You have mentioned that there is “a black shadow on the left brain which indicates an old stroke a few weeks before the cardiac arrest”.
Well, if that’s the case you and your family should have an indication on how well your Dad was functioning before he had the cardiac arrest, which is an indicator to which level of function he should be able to go back to.
Certainly, with your Dad being Diabetic, having sleep apnea, high blood pressure(hypertension) and kidney problems he was at higher risk to sustain both, a stroke and a cardiac arrest in the first place.
The health issues that your Dad has been experiencing before the stroke and the cardiac arrest are typical conditions that lead up to and increase the risk of sustaining a stroke and a cardiac arrest.
It’s good news that both CT’s, the CT of his brain and the CT of his chest are clear and only show the black shadow on the left side of the brain, indicating an old stroke.
Furthermore, besides the CT of the brain and the CT of the chest however, they also need to look into further testing your Dad’s heart and brain.
I.e. they need to follow up with an Echocardiogram(=Ultrasound of the heart) to determine where exactly and how much damage to the heart has been done. They may also do a TOE(=transoesophageal echocardiogram) which is an echocardiogram being performed through the Oesophagus to be as close to the heart as possible to make the diagnosis as accurate as possible.
This will determine the size and location of the damage to the heart and it’ll determine the ejection fraction(=measurement in determining how well your heart is pumping out blood and in diagnosing and tracking heart failure) of the heart.
From there on, treatment options such as the correct choosing of inotropes such as Noradrenaline, Adrenaline, Dobutamine, Milrinone and/or Levosimendan can be made.
Furthermore in significant heart failure, such as after cardiac arrest with no or minimal brain damage other treatment options such ECMO, LVAD and/or heart transplant may be explored.
Depending on where your Dad is currently being treated it might mean a referral to another more specialised ICU is being needed where such treatment options like ECMO, LVAD and/or heart transplant is available.
Now, given that your father was in cooling therapy for 72 hours you have to give your father time to “wake up”. Cooling therapy after cardiac arrest is currently best practice and the body, including the brain are being cooled down to 32° to 34° C (89.6° to 93.2° F) in order to minimise blood flow and protect vital body organ functions and it counteracts many of the destructive mechanisms of cardiac arrest.
During the cooling therapy, your Dad would have been heavily sedated on either Midazolam(Versed), Propofol(Diprivan) and on Morphine or Fentanyl. Therefore given the cardiac arrest, the stroke prior to the cardiac arrest, the cooling therapy and the induced coma you can expect a delay in your Dad “waking up”!
Related article/video:
If your Dad by now, after more than a week in ICU, after still being sedated is opening his eyes and then falls back to sleep he’s just at a normal stage during such a big and also life threatening event like a cardiac arrest.
Therefore, everything you have described and asked so far is nothing out of the ordinary and it’s nothing that is unusual in a situation after cardiac arrest.
Again, cooling therapy for 72 hours with some heavy sedation and induced coma to be able for the body to tolerate cooling down to 32° to 34° C (89.6° to 93.2° F), as well as ongoing lighter sedation to give the body and all major organs time to rest and heal is nothing unusual.
I can only imagine how stressed you and your family must feel by watching your Dad going through this, but rest assured that given that the CT of the brain is showing minimal signs of brain damage that you need to give your Dad time to rest, heal and “wake up” in his own time.
Related article/video:
You also need to keep in mind that with pre- hospital admission health issues like sleep apnea, diabetes and kidney issues there is a higher risk for your Dad to “wake up” slower after the induced coma.
Depending on how well your Dad is maintaining his blood pressure after the cardiac arrest, there is a risk of him going into kidney failure with his pre-medical kidney problems.
If the kidneys are not working 100%, there is also a higher risk of your Dad “waking up” slower after the induced coma, because almost all sedative drugs(Midazolam/Versed and Propofol/Diprivan) and opioid drugs(Morphine, Fentanyl) are excreted through the kidneys and if the kidneys are not functioning 100% you can expect a delay in “waking up”.
Therefore be patient for now, you, your family and your Dad are doing great in the bigger scheme of things.
Your Dad is alive, he survived a cardiac arrest and now he needs time to rest and heal and get out of ICU alive.
With his pre-medical condition of sleep apnea he may also need more time to get off the ventilator when coming out of the induced coma. Sleep apnee means he’ll stop breathing intermittently during sleep.
Whilst he’s on a ventilator in ICU, the ventilator will take care of any apneeic episodes however once off the ventilator he may need some NIV(Non-invasive ventilation) with a CPAP or BIPAP mask.
Here are some links to articles/videos that will help you clarify how “waking up” after an induced coma occurs
Related article/video:
You may also want to check out this article/video here as it relates to “waking up” after query or potential brain damage
Again Sarah, you, your family and your Dad are doing great! Give it time and be patient.
I know this is easier said than done. You probably feel like time stands still and it must feel like an eternity to you when you see your Dad like this.
As far as your Dad’s Pleural effusion goes that he’s having a chest drain for, know this.
It could well be a side effect from the cardio-pulmonary resuscitation efforts, as the chest would have been severely compressed during resuscitation and CPR.
Related:
Therefore, a pleural effusion(=is a condition in which excess fluid builds around the lung) is no surprise to me after cardiopulmonary resuscitation and CPR.
As long as they are draining this with a chest drain for few days, he should be fine and it should one his minor concerns.
Moving forward from here, your Dad needs to get out of the induced coma first, getting off any support that he’s on for his heart, I.e. Inotropes, slowly starting to get out of bed, go to a ward and then ideally go on to cardiac rehabilitation.
Give your Dad time, he’s doing great and be patient in his recovery!
I hope this helps Sarah, please let me know if I can help you with anything else or if you have any other questions.
Wishing you and your family all the very best!
Your friend!
Patrik
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care(it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!