What is Pneumonia?
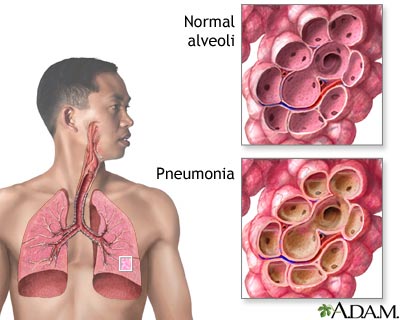
Pneumonia is a serious lung disorder and an inflammatory condition of the lung, leading to a number of Patients being admitted to Intensive Care—affecting primarily the microscopic air sacs known as alveoli. It is usually caused by infection with viruses or bacteria and less commonly other microorganisms, certain drugs and other conditions such as autoimmune diseases. This makes the absorption of Oxygen in the lungs very difficult and as a result the Patient with Pneumonia generally feels difficulties and an increased effort in breathing.
Typical symptoms include a cough, chest pain, fever, and difficulty breathing. Diagnostic tools include Chest X-ray and culture of the sputum. Vaccines to prevent certain types of pneumonia are available. Treatment depends on the underlying cause. Presumed bacterial pneumonia is treated with antibiotics. If the pneumonia is severe, the affected person is generally admitted to hospital.
Annually, pneumonia affects approximately 450 million people, seven percent of the world’s total, and results in about 4 million deaths. Although pneumonia was regarded by William Osler in the 19th century as “the captain of the men of death”,[ the advent of antibiotic therapy and vaccines in the 20th century has seen improvements in survival. Nevertheless, in developing countries, and among the very old, the very young and the chronically ill, Pneumonia remains a leading cause of death.
- What does the Respiratory System do?
- Signs& Symptoms
- What Happens in Intensive Care?
- How long will the Patient remain in Intensive Care?
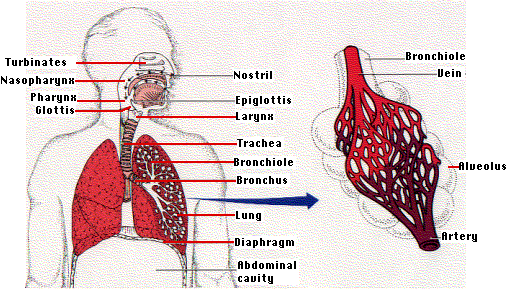
What does the Respiratory System do?
The respiratory system consists of the lungs, airways and blood vessels. The respiratory system inhales oxygen into the body and exchanges oxygen by removing carbon dioxide from the body. A normal breath requires a complex coordination between the nervous system (brain & spinal cord) and the muscles of breathing (including the diaphragm and muscles between the ribs).
Abnormal and or inadequate breathing can occur as a result of:
- An interruption to the nervous system (head injuries or spinal injuries for example)
- Barriers to the absorption of oxygen (eg fluid or secretions in the alveoli);
- Obstruction to the flow of gases through the lungs, both breathing in or out (eg asthma);
- Damage to the rib cage such as rib fractures or flail chest(in motor vehicle trauma for example);
- Pneumothorax(deflation of one part of the lung)
- Haemothorax(infiltration with blood to parts of the lung)
- Pain, which makes taking a normal breath difficult.
A number of respiratory conditions can result in respiratory failure and require Intensive Care or High dependency Unit admission. It is often that respiratory failure results in ventilation support (help with breathing). This support may be through the use of oxygen masks, BIPAP or Non- Invasive Ventilation(NIV) or via a Breathing Tube (endotracheal tube) and Ventilators (Breathing Machines)
Many respiratory conditions, including the above, can lead to admission to Intensive Care or High dependency Care Units. In those units oxygen and/or ventilator support may be initiated ranging from Oxygen Therapy via Oxygen mask to Non- Invasive Ventilation(NIV) or BIPAP ventilation or if the Patient’s condition deteriorates further a Breathing Tube (endotracheal tube) and mechanical ventilation on Ventilators (Breathing Machines) may be required.
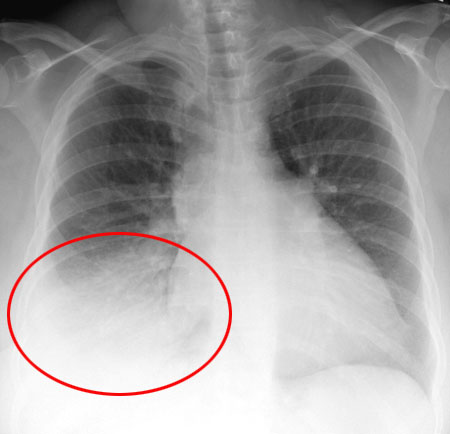 Chest x-ray showing pneumonia (circle) of the right middle lobe.
Chest x-ray showing pneumonia (circle) of the right middle lobe.
This image was found using a google search
Signs& Symptoms
If your loved one requires admission to a Critical Care area(Intensive Care or High dependency) for Pneumonia, it is because the Pneumonia shows signs and symptoms such as
- Productive cough
- fever
- Shortness of breath
- Increased Respiratory Rate(Tachypnoe)
- blue tinged skin
- decreased thirst
- convulsions
- persistent vomiting
- decreased level of consciousness
- Pneumonia caused by Legionella may occur with abdominal pain, diarrhea, or confusion
- Pneumonia caused by Streptococcus pneumoniae is associated with rusty colored sputum
- Pneumonia caused by Klebsiella may have bloody sputum often described as “currant jelly”.
- Bloody sputum (known as hemoptysis) may also occur with tuberculosis, Gram-negative Pneumonia, and lung abscesses as well as more commonly with acute bronchitis.
- Mycoplasma Pneumonia may occur in association with swelling of the lymph nodes in the neck, joint pain, or a middle ear infection.
- Viral Pneumonia presents more commonly with wheezing than does bacterial pneumonia.
What happens in Intensive Care?
If your loved one is admitted to Intensive Care for treatment of Pneumonia he or she has usually developed Respiratory Failure secondary to the Pneumonia and stabilisation of your loved one is paramount. Usually on admission to Intensive Care
- Your loved one will be closely monitored using a Bedside Monitors.
- Initially oxygen and respiratory support might be commenced via na oxygen mask or via Non- Invasive Ventilation(NIV) or BIPAP ventilation
- In Intensive Care if Non- Invasive ventilation is not sufficient, your loved one will very likely require a Breathing Tube (endotracheal tube) and mechanical ventilation on Ventilators (Breathing Machines)
- Frequent Chest X-rays and blood tests (Blood& Pathology tests in Intensive Care)especially arterial blood gases (ABGs) will be performed regularly
- Infusion pumps are administering drugs to support your loved ones blood pressure and haemodynamic system, as well as intravenous fluids may be administered via a central venous catheter/ CVC(Central Venous Lines)
- An NG Tube (Nasogastric Tubes) is usually inserted into your loved ones stomach, in order to commence nutrition or to remove fluids
- Urine Output is usually measured hourly, after insertion of a Urinary Catheter
- The cause of the infection is investigated and drug treatment will differ according to the suspected or known organism.
- Management of your loved one is dependent on how critically ill they have become.
- Treatment includes oxygen and antibiotics to fight the infection.
How long will your loved one remain in Intensive Care?
How long your loved one requires therapy in Intensive Care depends largely on the severity of the Pneumonia and on your loved ones immune system to fight the infection. It also depends on how well the Antibiotic therapy counteracts the infection. Another factor impacting on your loved ones length of stay in Intensive Care is whether and how long they need Non- Invasive Ventilation(NIV) or BIPAP ventilation. If Non-Invasive BIPAP ventilation is not sufficient and your loved one requires a Breathing Tube (endotracheal tube) and mechanical ventilation on Ventilators (Breathing Machines) the length of stay or length of time usually goes up and may exceed 3-4 days, sometimes up to two weeks.
Most Patients admitted to Intensive Care with Pneumonia fully recover, but in some severe cases few Patients may die.
Related article/video:
HOW LONG IS MY LOVED ONE GOING TO STAY IN INTENSIVE CARE WITH PNEUMONIA?
Any Questions?
Of course, if you have any questions or concerns, please discuss them with the ICU nurses and doctors.
All Intensive Care interventions and procedures carry a degree of potential risk even when performed by skilled and experienced staff. Please discuss these issues with the medical and nursing staff who are caring for your loved one.
The information contained on this page is general in nature and therefore cannot reflect individual patient variation. It is meant as a back up to specific information which will be discussed with you by the Doctors and Nurses caring for your loved one. INTENSIVE CARE HOTLINE attests to the accuracy of the information contained here BUT takes no responsibility for how it may apply to an individual Patient. Please refer to the full disclaimer.
How can you have PEACE OF MIND, control, power and influence whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below! In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care! Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below!
In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care!
In your FREE reports you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 “killer” tips& strategies helping you to get on the right path to PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘BEHIND THE SCENES’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care(it’s not what you think)
Make sure you also check out our “blog” section for tips& strategies and also check out our “your questions answered” section where we answer your questions or send me an email to [email protected] with your questions!
Sincerely, your Friend
Patrik Hutzel
Related articles:
- What is an induced coma and why is my critically ill loved one in an induced coma?
- How long is a Patient kept on a BIPAP machine in Intensive Care?


