What is Multi-trauma or Polytrauma?
Polytrauma or multiple trauma is a medical term describing the condition of a person who has been subjected to multiple traumatic injuries, such as a serious head injury, multiple fractures in addition to a serious burn, affecting multiple body systems and organs. The term is generic, and has been in use for a long time for any case involving multiple traumata. Generally, the more body parts and body systems affected, the more serious the condition.
Polytraumas are often associated with motor vehicle accidents. This is because car accidents often occur at a high velocities causing multiple injuries. On admission to hospital any trauma Patient should immediately undergo x-ray diagnosis of their cervical spine, chest and their pelvis, commonly known as a ‘trauma series’, to ascertain possible life threatening injuries. Examples would be a fractured cervical vertebra, a severely fractured pelvis, or a haemothorax. Once the initial survey is complete, x-rays can be taken of the limbs to assess for other possible fractures. It is also quite common in severe trauma for patients to go straight to CT or a surgery theatre if they require emergency treatment.
ECMO(Extracorporeal Membrane Oxygenation ) can be effective in treating some polytrauma patients with pulmonary or cardiopulmonary failure.
A retrospective study of 93 children (average age of 8.0 +/- 4.1 years) with polytrauma and at least one major musculoskeletal injury showed that 80% of the incidents had been caused in this way (motor vehicle accident).
- Trauma
- What happens in Intensive Care?
- What are the complications of multi-trauma?
- How long will your loved one remain in the ICU?
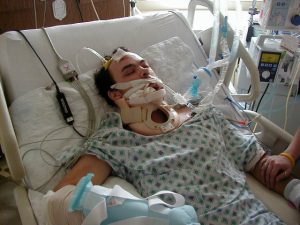

Trauma
- Trauma is usually categorised as blunt or penetrating. Blunt trauma refers to physical trauma caused to a body part, either by impact, injury or physical attack; the latter usually being referred to as blunt force trauma. The term refers to the initial trauma, from which develops more specific types such as contusions, abrasions, lacerations, and/or bone fractures. Blunt trauma is contrasted with penetrating trauma, in which an object such as a bullet enters the body.Assessment and diagnosis of blunt injuries are more difficult than of penetrating injuries, because blunt injuries are not usually internal, and not obvious. Penetrating trauma is an injury that occurs when an object pierces the skin and enters a tissue of the body, creating an open wound. In blunt, or non-penetrating trauma, there may be an impact, but the skin is not necessarily broken. The penetrating object may remain in the tissues, come back out the way it entered, or pass through the tissues and exit from another area.An injury in which an object enters the body or a structure and passes all the way through is called a perforating injury, while penetrating traumaimplies that the object does not pass through. Perforating trauma is associated with an entrance wound and an often larger exit wound. Penetrating trauma can be caused by a foreign object or by fragments of a broken bone. Usually occurring in violent crime or armed combat, penetrating injuries are commonly caused by gunshots and stabbings.Penetrating trauma can be serious because it can damage internal organs and presents a risk of shock and infection. The severity of the injury varies widely depending on the body parts involved, the characteristics of the penetrating object, and the amount of energy transmitted to the tissues. Assessment may involve X-rays or CT scans, and treatment may involve surgery, for example to repair damaged structures or to remove foreign objects.
- Trauma is the sixth leading cause of death worldwide, accounting for 10% of all mortality’s, and is therefore a serious public health problem with significant social and economic costs. According to the World Health Organization (WHO) in the year 2000, 5 million people died of injuries, accounting for 10% of global annual mortality. That same year, 12% of the global burden of disease resulted from injury. Over 90% of the world’s trauma mortality occurs in low- and middle-income nations, with those in Eastern Europe having the highest rates. Almost 50% of those who die are between 15 and 44 years of age, with males accounting for twice as many deaths as females. Violence—self-inflicted, interpersonal, and war-related—accounts for half of trauma mortality, with 1.6 million deaths in the year 2000. Road traffic accounts for the next largest proportion, roughly 1.2 million deaths, per year, 2.1% of overall mortality. An additional 20 to 50 million people are injured annually in road traffic incidents. Though most of the world’s trauma deaths occurs in developing countries, trauma is a significant cause of injury and death in industrialised nations as well. Road traffic accidents, including motor vehicle, motor bikes and pedestrians are the most common causes of trauma requiring admission into Intensive Care.
What happens in the Intensive Care Unit?
- Your loved one with Multi trauma will be admitted to Intensive Care if they have suffered a severe injury. On most occasions your loved one will be admitted to the Intensive Care following surgery. Once in ICU your loved one will be under the care of the Intensive Care team with the surgical team reviewing your loved one on a regular basis.
- Your loved one is continuously monitored with a Bedside Monitors– Your loved ones vital signs such as Blood pressure is usually displayed continuously on the bedside monitor via an Arterial Catheter. Your loved ones Heart, Heart rhythm(ECG), temperature and breathing rate is continuously monitored and displayed on the monitor. Oxygen levels are continuously monitored by an oxygen saturation probe attached to the finger or to the ear. Furthermore oxygen levels are intermittently checked with ABG’s(Arterial Blood Gases), where blood is drawn out of the Arterial Catheter and tested immediately via a Blood Gas Analyser.
- Your loved ones breathing will be supported by additional oxygen via an oxygen mask, or Non- Invasive Ventilation(NIV) or BIPAP ventilation, however your loved one may be on a Ventilator (Breathing Machine) and have a Breathing Tube (Endotracheal tube) inserted into their airway. Most Multi- Traumas are in an induced Coma and therefore require mechanical ventilation with a Ventilator (Breathing Machine). Multi Trauma can also lead to Tracheostomy insertion Tracheostomy ventilation
- If your loved one has a head injury or brain injury he or she may require Intracranial Pressure Monitoring, which basically monitors the pressure in your loved ones head
- Your loved one will be receiving intravenous fluids via several intravenous cannula’s or Central Venous Lines(central line or CVC). A Urinary Catheter is used to monitor urine output and a Nasogastric Tubes will be used to rest the intestine if this has been injured or if your loved one requires ventilation.
- You can expect your loved one to have frequent Chest X-rays and blood tests(Blood& Pathology tests in Intensive Care) especially arterial blood gases (ABGs)
- Your loved one may have drains coming out of the Chest if the Chest has been injured (Under Water Seal Drain & Chest Tube)
- Anti-thrombotic stockings will be applied to guard against the development of a deep vein thrombosis (DVT) in the lower limbs. A sequential compression device may also be used. Pain medication will be given to ensure they are as pain free as possible. Nutrition will be started as early as possible. Feeding via a nasogastric tube is preferred. However if this is not possible, your loved one will be fed intravenously with TPN(Total Parenteral Nutrition).
What are the complications of multitrauma?
- Pain is the most often cited problem associated with Multitrauma. Therefore you may find that your loved one has high doses of pain killers infused, often strong opiates such as Morphine, Fentanyl or Remifentanyl
- Bleeding(Hemorrhage) may arise after multitrauma and it is therefore a priority to constantly check and test for bleeding
- Infection and Sepsis are very common in Multitrauma Patients, due to the nature of open wounds
- Multi organ failure- trauma to multiple organs, including all major organs brain, heart, lungs, liver and kidneys may cause some major organs to fail. This is one of the reasons why your loved one may require mechanical ventilation, as well as intravenous medication to support your loved ones heart and blood pressure with inotropic medication. Furthermore, if the kidneys fail your loved one may require a Dialysis Catheter and a Dialysis Machines for Renal Replacement Therapy or Haemodialyisis
- If your loved one is to stay in Intensive Care for many months, due to ventilator dependency and is medically stable, also check out this site for more information www.intensivecareathome.com.au as home care with a much better Quality of Life for your loved one and for the Family could be an option.
How long will your loved one remain in Intensive Care?
Your loved ones stay in ICU may vary from a few days to a few months, depending on what their injuries are. Please ask the ICU nurse or doctor if you have any questions.
Any Questions?
Of course, if you have any questions or concerns, please discuss them with the ICU nurses and doctors.
All Intensive Care interventions and procedures carry a degree of potential risk even when performed by skilled and experienced staff. Please discuss these issues with the medical and nursing staff who are caring for your loved one.
The information contained on this page is general in nature and therefore cannot reflect individual Patient variation. It is meant as a back up to specific information which will be discussed with you by the Doctors and Nurses caring for your loved one. INTENSIVE CARE HOTLINE attests to the accuracy of the information contained here BUT takes no responsibility for how it may apply to an individual Patient. Please refer to the full disclaimer
How can you have PEACE OF MIND, control, power and influence whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below! In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care! Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below!
In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care!
In your FREE reports you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 “killer” tips& strategies helping you to get on the right path to PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘BEHIND THE SCENES’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care(it’s not what you think)
Make sure you also check out our “blog” section for tips& strategies and also check out our “your questions answered” section where we answer your questions or send me an email to [email protected] with your questions!
Sincerely, your Friend
Patrik Hutzel
Related Articles:
- What is an induced coma and why is my critically ill loved one in an induced coma?
- The 3 most dangerous mistakes that you are making but you are unaware of, if your loved one is a critically ill Patient in Intensive Care
- How to always achieve your goals whilst your loved one is critically ill in Intensive Care
- Why you must make up your own mind about your critically ill loved one’s situation in Intensive Care even if you’re not a doctor or a nurse!
- Follow this proven 5 step process on how to be in control and influential if your loved one is a long-term Patient in Intensive Care
- How to take control if your loved one has a severe brain injury and is critically ill in Intensive Care
- How long does it take to wake up from a Traumatic brain injury or severe head injury?
- What you need to do if your loved one in Intensive Care is brain dead or is considered for organ donation
- What is an induced coma and why is my critically ill loved one in an induced coma?
- How long can a breathing tube or an endotracheal tube can stay in?
- How long should a Patient be on a ventilator before having a Tracheostomy?
- Why does my loved one need a Tracheostomy in Intensive Care?
- How long is a Patient kept on a BIPAP machine in Intensive Care?
- How to quickly take control and have real power and influence if your loved one is critically ill in Intensive Care
- Tracheostomy and weaning off the ventilator in Intensive Care, how long can it take?
- My sister has been in ICU for 21 weeks with Tracheostomy and still ventilated. What do we need to do?
- Severe lung failure and my aunty is not expected to survive…
- Be more selfish if your loved one is critically ill in Intensive Care
- 3 quick steps on how to position and prepare yourself well mentally, whilst your loved one is critically ill in Intensive Care
- How to get what you want whilst your loved one is critically ill in Intensive Care
- 5 steps to become a better negotiator if your loved one is critically ill in Intensive Care
- 5 Ways to have control, power and influence while your loved one is critically ill in Intensive Care
- How to make sure that your values and beliefs are known whilst your loved one is critically ill in Intensive Care
- How to make sure that “what you see is always what you get” whilst your loved one is critically ill in Intensive Care
- What the doctors and the nurses behaviour in Intensive Care is telling you about the culture in a unit
- Family Meetings in Intensive Care or the Elephant in the Room
- What you need to do if your loved one is dying in Intensive Care(part one)
- What you need to do if your loved one is dying in Intensive Care(part two)
- Intensive Care at its best?
- How INTENSIVECAREHOTLINE.COM Can Help You
- What you and your Family need to do if your critically ill loved one is very sick in Intensive Care and faces an uncertain future
- How long can somebody stay in Intensive Care?
- My Family can’t agree on what’s best for my sister in Intensive Care…Help!
- My husband is dying in Intensive Care, but we need more time…
- My mother sustained serious brain damage after a stroke and she now is in multi- organ failure


