What is a liver transplantation?
Liver transplantation or hepatic transplantationis the replacement of a diseased liver with a healthy liver from another person (allograft). The most commonly used technique is orthotopic transplantation, in which the native liver is removed and replaced by the donor organ in the same anatomic location as the original liver. Liver transplantation nowadays is a well accepted treatment option for end-stage liver disease and acute Liver Failure. Typically three surgeons and two anesthesiologists are involved, with up to four supporting nurses. The surgical procedure is very demanding and ranges from 4 to 18 hours depending on outcome. Numerous anastomoses(connections of blood vessels) and sutures, and many disconnections and re-connections of abdominal and liver(hepatic) tissue, must be made for the transplant to succeed, requiring an eligible recipient and a well-calibrated live or cadaveric donor match. By any standard, liver(hepatic) transplantation is a major surgical procedure with an appreciable degree of risk.
- Indications for liver transplantation
- What does the liver do?
- What happens during liver transplantation?
- What happens in Intensive Care?
- Immunosuppression
- Complications
- How long is my loved one going to stay in Intensive Care?
- Links
Indications for Liver transplantation
Liver transplantation is potentially applicable to any acute or chronic condition resulting in irreversible liver dysfunction, provided that the recipient does not have other conditions that will preclude a successful transplant. Uncontrolled metastatic cancer outside liver, active drug or alcohol abuse and active septic infections are absolute contraindications. While infection with HIV was once considered an absolute contraindication, this has been changing recently. Advanced age and serious heart, pulmonary or other disease may also prevent transplantation (relative contraindications). Most liver transplants are performed for chronic liver diseases that lead to irreversible scarring of the liver, or cirrhosis of the liver.
What does the Liver do?
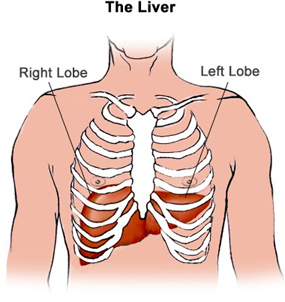
The liver is the second largest organ in the body, sitting under the diaphragm and lungs. There are two lobes or sections of the liver, the right and the left lobe. The right lobe is six times larger than the left. The liver is made up of many liver cells called hepatocytes. The liver is an important organ in the body and is responsible for a number of essential functions.
The liver
- Filters the blood and breaks down toxins such as drugs and alcohol.
- Processes old blood cells and stores iron.
- Helps to maintain normal blood sugar level.
- Produces the majority of clotting factors.
- Produces and maintains normal levels of protein in the blood.
- Assists in resisting infections by producing immune factors and removing bacteria from the blood.
- Plays a central role in fat and protein metabolism.
What happens during Liver transplantation?
Virtually all liver transplants are done in an orthotopic fashion, that is, the native liver is removed and the new liver is placed in the same anatomic location. The transplant operation can be conceptualized as consisting of the hepatectomy (liver removal) phase, the anhepatic (no liver) phase, and the postimplantation(new liver) phase. The operation is done through a large incision in the upper abdomen(Laparotomy). The hepatectomy involves division of all ligamentous attachments to the liver, as well as the common bile duct, hepatic artery, hepatic vein and portal vein. Usually, the retrohepatic portion of the inferior vena cava is removed along with the liver, although an alternative technique preserves the recipient’s vena cava (“piggyback” technique).
The donor’s blood in the liver will be replaced by an ice-cold organ storage solution, such as until the new(allograft) liver is implanted. Implantation involves anastomoses (connections) of the inferior vena cava, portal vein, and hepatic artery. After blood flow is restored to the new liver, the biliary (bile duct) anastomosis is constructed, either to the recipient’s own bile duct(gall bladder duct) or to the small bowels. The surgery usually takes between five and six hours, but may be longer or shorter due to the difficulty of the operation and the experience of the surgeon.
The large majority of liver transplants use the entire liver from a non-living donor for the transplant, particularly for adult recipients. A major advance in pediatric liver transplantation was the development of reduced size liver transplantation, in which a portion of an adult liver is used for an infant or small child. Further developments in this area included split liver transplantation, in which one liver is used for transplants for two recipients, and living donor liver transplantation, in which a portion of a healthy person’s liver is removed and used as the allograft. Living donor liver transplantation for pediatric recipients involves removal of approximately 20% of the liver.
Further advance in liver transplant involves only resection of the lobe of the liver involved in tumors and the tumor-free lobe remains within the recipient. This speeds up the recovery and the patient stay in the hospital quickly shortens to within 5–7 days.
What happens in the Intensive Care Unit?
As Patients with multiple comorbidities and organ dysfunction are undergoing Liver transplants, an appropriate Intensive Care management is required to support prompt graft and liver recovery and prevent complications.
After the surgery for Liver Transplant has been completed your loved one is admitted to the Intensive Care/ Critical care Unit and your loved one
- will require monitoring using a Bedside Monitors and an Arterial Catheter(Arterial Line)
- You can expect your loved one to have frequent Chest X-rays and blood tests(Blood& Pathology tests in Intensive Care) especially arterial blood gases (ABGs)
- Full ventilation using a Ventilators(Breathing Machine) and a Breathing Tube (endotracheal tube) will usually be required to improve and maintain the oxygen delivery. Full ventilation support may last from few hours to a few days. In case your loved one is unstable, he or she will require ongoing ventilation, sometimes Tracheostomy ventilation
- Sedation such as Propofol, Midazolam, Morphine or Fentanyl may be used if your loved one is in an induced coma
- Usually, after your loved one has been stabilised he or she may be taken off full ventilatory support and after full ventilation support has been discontinued, oxygen and respiratory support might be commenced via an oxygen mask or via Non- Invasive Ventilation(NIV) or BIPAP ventilation
- Infusion pumps are administering drugs to support your loved ones blood pressure and haemodynamic system, as well as intravenous fluids may be administered via a central venous catheter/ CVC(Central Venous Lines)
- An NG Tube (Nasogastric Tubes) is usually inserted into your loved ones stomach, in order to commence nutrition or to remove fluids
- Urine Output is usually measured hourly, after insertion of a Urinary Catheter
- Especially significant blood loss during surgery usually requires massive amounts of intravenous fluids and blood products to preserve cardiac output and organ perfusion
A functioning transplanted liver is almost always associated with organ system recovery, resulting in a new life for your loved one. However, in the unfortunate event of graft dysfunction, the unavoidable development of multi-organ failure will require an enhanced level of critical care support and a prolonged stay in ICU.
Immunosuppression
Like most other organ transplants, a liver transplant will be rejected by the recipient unless immunosuppressive(reduces the activation of the immune system) drugs are used. The immunosuppressive regimens for all solid organ transplants are fairly similar, and a variety of agents are now available. Most liver transplant recipients receive corticosteroids(steroids) plus a calcineurin inhibitor such as tacrolimus or ciclosporin plus a purine antagonist such as mycophenolate. Clinical outcome is better with tacrolimus than with cyclosporin during the first year of liver transplantation. If your loved one has a pre-medical condition such as active hepatitis B, high doses of hepatitis B immunoglubins are administrated in liver transplant Patients. Liver transplantation is unique in that the risk of chronic rejection also decreases over time, although the great majority of recipients need to take immunosuppressive medication for the rest of their lives. It is possible to be slowly taken off anti rejection medication but only in certain cases.

Complications
Despite substantial technological, medical and surgical advances and improvement in recent years, Liver Transplantation remains a complex procedure that is accompanied by significant morbidity. Frequent complications on both the graft and the organ systems arise because of multiple, and sometimes unavoidable adverse events.
The main complications are
- Primary graft failure, which is characterized by the incapacity of the new graft to maintain the recipient metabolic homeostasis(chemical balance), and is associated with a high risk of death without an emergency retransplantation
- Biliary complications have been described as the “Achilles heel” of liver transplantation. Biliary leaks are a common consequence of necrosis(tissue death) at the surgical anastomosis, technical errors or biliary tract ischemia(lack of oxygen). They are very frequent in living donor liver transplantation. Lack of bile outflow through a drainage, an increase of cholestatic(gall) enzymes are indicative of a biliary complication. Ultrasound and/or abdominal CT scans may confirm the diagnosis. The leak may resolve itself conservatively or may require treatment. Treatment options include biliary stenting or percutaneous transhepatic cholangiography with external drainage, or surgical repair
- Acute rejection normally occurs 7-14 d after the operation but can manifest earlier or much later. Hyperacute graft rejection is very rare in liver transplantation and is determined by preformed antibodies. Rejection is associated with graft dysfunction and negatively affects graft survival. Treatment depends on the severity of the rejection and the underlying diagnosis of the Patient. Mild rejection may respond to an increase in baseline immunosuppressive doses, steroids, the use of mycophenolate and/or a switch to tacrolimus if the Patient was on cyclosporine. More severe rejections require repeated steroid boluses and/or antilymphocyte globulin. Rarely does acute rejection require retransplantation
- Post operative bleeding and coagulopathy. Poor graft function, imperfect hemostasis, slippage of a tie, hypersplenism, hypocalcaemia(low calcium, levels) and dilution may lead to bleeding which necessitates transfusion or surgical re-exploration. Intra-abdominal and wound “oozing” in the first post-operative hours may also result from heparin release from the implanted graft along with hyperfibrinolysis. The risk of bleeding is increased by thrombocytopenia, mainly caused by low platelets levels in the blood activation-consumption and sequestration following graft reperfusion and platelet-associated antibody production. Other causes of thrombocytopenia include viral infection and treatment with antiviral therapy. Thrombocytopenia usually regresses within two weeks, but in some individuals it lasts longer due to persistent splenomegaly(enlarged spleen)
- Neurological complications. The most frequent complications are encephalopathy, brain hemorrhage, and Seizures. Patients with neurologic symptoms prior to transplantation are at greater risk for post-operative neurologic disturbances. Seizures are the second most common neurological complications reported in liver transplanted Patients. Seizures may be a consequence of factors including stroke, metabolic(chemical) disturbances, electrolyte disorders, drug toxicity, previous history of epileptic seizures, central nervous system infection and are often preceded by some degree of encephalopathy
- Renal dysfunction. Sometimes Patients undergoing a liver -transplant are at a higher risk to develop Acute Kidney(Renal) Failure. Like with many other admissions to Intensive Care, the critical clinical state before transplant, intraoperative hemodynamic disturbances, massive transfusion, and many post-operative adverse events, such as infections, surgical re-exploration, and radiological investigations are frequently involved in the development of acute renal failure. Your loved one may require regular Lasix or Lasix infusion or he or she may require a Dialysis Catheter for Haemodialysis(Dialysis Machines)
How long is my loved one going to stay in Intensive Care?
Length of stay in Intensive Care varies from few days, to sometimes weeks or months. Patients are different and therefore it is difficult to ascertain an exact time period.
Links
USA Liver foundation http://www.liverfoundation.org/abouttheliver/info/transplant/
http://www.transplant.org.au/Why-people-need-transplants.html Transplant Australia
http://www.organdonor.gov U.S. Government Information on Organ and Tissue Donation and Transplantation
http://www.organdonation.nhs.uk/ Organ donation in the United Kingdom
http://www.nhs.uk/conditions/Liver-transplant/Pages/Introduction.aspx Liver transplant in the NHS in the UK
Any Questions?
Of course, if you have any questions or concerns, please discuss them with the ICU nurses and doctors.
All Intensive Care interventions and procedures carry a degree of potential risk even when performed by skilled and experienced staff. Please discuss these issues with the medical and nursing staff who are caring for your loved one.
The information contained on this page is general in nature and therefore cannot reflect individual Patient variation. It is meant as a back up to specific information which will be discussed with you by the Doctors and Nurses caring for your loved one. INTENSIVE CARE HOTLINE attests to the accuracy of the information contained here BUT takes no responsibility for how it may apply to an individual Patient. Please refer to the full disclaimer.
Related Articles:
- How long can a breathing tube or an endotracheal tube can stay in?
- How long should a Patient be on a ventilator before having a Tracheostomy?
- How long is a Patient kept on a BIPAP machine in Intensive Care?
- What is an induced coma and why is my critically ill loved one in an induced coma?
- The 3 most dangerous mistakes that you are making but you are unaware of, if your loved one is a critically ill Patient in Intensive Care
- How to always achieve your goals whilst your loved one is critically ill in Intensive Care
- Why you must make up your own mind about your critically ill loved one’s situation in Intensive Care even if you’re not a doctor or a nurse!
- Follow this proven 5 step process on how to be in control and influential if your loved one is a long-term Patient in Intensive Care
- How to quickly take control and have real power and influence if your loved one is critically ill in Intensive Care
- Why does my loved one need a Tracheostomy in Intensive Care?
- Tracheostomy and weaning off the ventilator in Intensive Care, how long can it take?
- My sister has been in ICU for 21 weeks with Tracheostomy and still ventilated. What do we need to do?
- Severe lung failure and my aunty is not expected to survive…
- Be more selfish if your loved one is critically ill in Intensive Care
- 3 quick steps on how to position and prepare yourself well mentally, whilst your loved one is critically ill in Intensive Care
- How to get what you want whilst your loved one is critically ill in Intensive Care
- How to stay positive if your loved one is critically ill in Intensive Care
- 5 steps to become a better negotiator if your loved one is critically ill in Intensive Care
- 5 Ways to have control, power and influence while your loved one is critically ill in Intensive Care
- How to make sure that your values and beliefs are known whilst your loved one is critically ill in Intensive Care
- How to make sure that “what you see is always what you get” whilst your loved one is critically ill in Intensive Care
- What the doctors and the nurses behaviour in Intensive Care is telling you about the culture in a unit
- How long does it take to wake up from a Traumatic brain injury or severe head injury
- How to take control if your loved one has a severe brain injury and is critically ill in Intensive Care
- Family Meetings in Intensive Care or the Elephant in the Room
- What you need to do if your loved one is dying in Intensive Care(part one)
- What you need to do if your loved one is dying in Intensive Care(part two)
- Intensive Care at its best?
- How INTENSIVECAREHOTLINE.COM Can Help You
- What you and your Family need to do if your critically ill loved one is very sick in Intensive Care and faces an uncertain future
- How long can somebody stay in Intensive Care?
- My Family can’t agree on what’s best for my sister in Intensive Care…Help!
- My husband is dying in Intensive Care, but we need more time…
- My mother sustained serious brain damage after a stroke and she now is in multi- organ failure


