What is Guillain-Barré Syndrome?
Guillain–Barré syndrome (GBS) is an acute polyneuropathy, a disorder affecting the peripheral nervous system. Ascending paralysis, weakness beginning in the feet and hands and migrating towards the trunk, is the most typical symptom, and some subtypes cause change in sensation or pain as well as dysfunction of the autonomic nervous system. It can cause life-threatening complications, in particular if the respiratory muscles are affected or if there is autonomic nervous system involvement. The disease is usually triggered by an infection.
The diagnosis is usually made by nerve conduction studies and with studies of the cerebrospinal fluid. With prompt treatment by intravenous immunoglobulins or plasmapheresis, together with supportive care, the majority will recover completely. Guillain–Barré syndrome is rare, at 1–2 cases per 100,000 people annually, but is the most common cause of acute non-trauma-related paralysis in the world. The syndrome is named after the French physicians Georges Guillain and Jean Alexandre Barré, who described it in 1916.
GBS is an autoimmune disorder. Autoimmune disorders happen when the defence system of the body (immune system), mistakes the person’s own cells/tissues as foreign, and begins to attack them. In GBS, the immune system attacks the peripheral nervous system and starts to destroy the myelin sheath that surrounds the nerves.
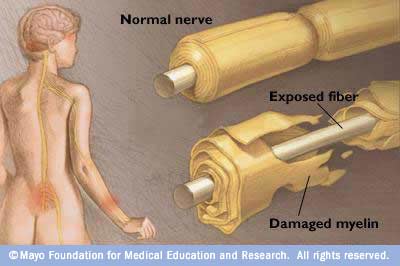
Guillain-Barre syndrome destroys the protective covering of the peripheral nerves (myelin sheath), preventing the nerves from transmitting signals to the brain. Image found at mayoclinic.com
- What causes Guillain Barré Syndrome?
- Signs and symptoms
- What happens in the ICU?
- How long will your loved one remain in ICU?
What causes Guillain-Barré Syndrome?
All forms of Guillain–Barré syndrome are autoimmune diseases, due to an immune response to foreign antigens (such as infectious agents) that is mistargeted at host nerve tissues instead, a phenomenon called molecular mimicry. The targets of such immune attack are thought to be gangliosides, compounds naturally present in large quantities in human peripheral nerve tissues. The most common antecedent infection is the bacterium Campylobacter jejuni followed by cytomegalovirus (CMV). However, 60% of cases do not have a known cause. Some cases may be triggered by the influenza virus, or by an immune reaction to the influenza virus.
The end result of this autoimmune attack on the peripheral nerves is damage to the myelin, the fatty insulating layer of the nerve, and a nerve conduction block, leading to muscle paralysis that may be accompanied by sensory or autonomic disturbances.
In mild cases, nerve axon (the long slender conducting portion of a nerve) function remains intact and recovery can be rapid if remyelination occurs. In severe cases, axonal damage occurs, and recovery depends on the regeneration of this important tissue. Approximately 80% of patients have myelin loss; in the remaining 20%, the pathological hallmark is axon loss.
Guillain–Barré, unlike disorders such as multiple sclerosis (MS) and Lou Gehrig’s disease (ALS), is a peripheral nerve disorder and does not in general cause nerve damage to the brain or spinal cord.
The exact cause of GBS is unknown. However, the autoimmune reaction that causes the nerve damage is usually triggered by an infection, such as a cold, sore throat or a stomach virus. It may also be related to having an immunisation, childbirth, or surgery. GBS is not contagious.
Signs and symptoms
The disorder is characterized by symmetrical weakness that usually affects the lower limbs first, and rapidly progresses in an ascending fashion. Patients generally notice weakness in their legs, manifesting as “rubbery legs” or legs that tend to buckle, with or without numbness or tingling. As the weakness progresses upward, usually over periods of hours to days, the arms and facial muscles also become affected. Frequently, the lower cranial nerves may be affected, leading to bulbar(eyeballs) weakness, oropharyngeal dysphagia (drooling, or difficulty swallowing and/or maintaining an open airway) and respiratory(breathing) difficulties. Most Patients require hospitalization and about 30% require ventilatory assistance for treatment of Type II respiratory failure. Facial weakness is also common.
Sensory loss, if present, usually takes the form of loss of position sense and areflexia (complete loss of deep tendon reflexes), an important feature of GBS. Loss of pain and temperature sensation is usually mild. In fact, pain is a common symptom in GBS, presenting as deep aching pain, usually in the weakened muscles, which Patients compare to the pain from overexercising. These pains are self-limited and may be treated with standard analgesics. Bladder dysfunction may occur in severe cases but is usually transient.
In severe cases of GBS, loss of autonomic function is common, manifesting as wide fluctuations in blood pressure, orthostatic hypotension (a fall in blood pressure on standing, leading to an increased risk of collapse), and cardiac arrhythmia’s.
Acute paralysis in Guillain–Barré syndrome may be related to sodium channel blocking factor in the cerebrospinal fluid (CSF). Significant issues involving intravenous salt and water administration may occur unpredictably in this patient group, resulting in SIADH(syndrome of immoderate antidiuresis), a cause of low sodium levels in the blood.
- Varying degree of muscle weakness and paralysis affecting both sides of the body
- Jerky, uncoordinated movements
- Numbness
- Muscle aches, muscle spasm, pains or cramps
- Abnormal sensations such as tingling, vibrations
- Blurred vision
- Dizziness
- Difficulty breathing
Tests and diagnosis
The diagnosis of GBS usually depends on findings such as rapid development of muscle paralysis, areflexia, absence of fever, and a likely inciting event. Cerebrospinal fluid analysis (through a lumbar spinal puncture) and electrodiagnostic tests of nerves and muscles (such as nerve conduction studies) are common tests ordered in the diagnosis of GBS.
In cerebrospinal fluid, characteristic findings include albumino-cytological dissociation. As opposed to infectious causes, this is an elevated protein level (100–1000 mg/dL), without an accompanying increased cell count (absence of pleocytosis). A sustained increased white blood cell count may indicate an alternative diagnosis such as infection.
Electromyography (EMG) and nerve conduction studies (NCS) may show prolonged distal latencies, conduction slowing, conduction block, and temporal dispersion of compound action potential in demyelinating cases. F waves and H-reflexes may be prolonged or absent. Needle EMG is frequently normal in acute cases. Reduced, neuropathic recruitment in weak muscles can be seen. Fibrillations will be seen on needle EMG if there is some axonal injury after 3 to 4 weeks. In primary axonal damage, the findings include reduced amplitude of the action potentials without conduction slowing.
How is Guillain-Barré Syndrome treated?
Supportive care is the cornerstone of successful management in the acute patient. Of greatest concern is respiratory failure due to paralysis of the diaphragm, the muscle most important for breathing. Intubation may be needed when there is evidence of impending failure of the muscles of breathing.
Subsequent treatment consists of attempting to reduce the body’s attack on the nervous system, either by plasmapheresis, filtering antibodies out of the blood stream, or by administering intravenous immunoglobulins (IVIg), to neutralize harmful antibodies and inflammation causing disease. These two treatments are equally effective and a combination of the two is not significantly better than either alone. Glucocorticoids have not been found to be effective in GBS. Treatment is usually begun as soon as the diagnosis is made. Plasmapheresis hastens recovery when used within 4 weeks of the onset of symptoms. IVIg has equivalent efficacy to plasmapheresis when started within 2 weeks of the onset of symptoms, and has fewer complications. IVIg is usually used first because of its ease of administration and safety profile. The use of intravenous immunoglobulins is not without risk, occasionally causing hepatitis, or in rare cases, renal failure if used for longer than five days.
Following the acute phase, treatment often consists of rehabilitation with the help of a multidisciplinary team to focus on improving activities of daily living (ADLs). Occupational therapists may offer equipment (such as wheelchair and special cutlery) to help your loved one achieve ADL independence. Physiotherapists assist to correct functional movement, avoiding harmful compensations that might have a negative effect in the long run. There is also some evidence supporting physiotherapy in helping patients with Guillain–Barré syndrome regain strength, endurance, and gait quality, as well as helping them prevent contractures, bedsores, and cardiopulmonary difficulties. Speech and language therapists help regain speaking and swallowing ability, especially if your loved one requires Intubation and mechanical ventilation(Ventilators (Breathing Machines) or received a Tracheostomy.
Most Patients diagnosed with Guillain–Barré syndrome, do fully recover, however it can sometimes take many months to years.
What happens in the Intensive Care Unit?
- Initially oxygen and respiratory support might be commenced via na oxygen mask or via Non- Invasive Ventilation(NIV) or BIPAP ventilation
- Full ventilation using a Ventilators(Breathing Machine) and a Breathing Tube (endotracheal tube) will usually be required to improve and maintain the oxygen delivery
- Sedation may be used if your loved one is in an induced coma
- Your loved one will require monitoring using a Bedside Monitors and an Arterial Catheter(Arterial Line)
- You can expect your loved one to have frequent Chest X-rays and blood tests(Blood& Pathology tests in Intensive Care) especially arterial blood gases (ABGs)
- Infusion pumps are administering drugs to support your loved ones blood pressure and haemodynamic system, as well as intravenous fluids may be administered via a central venous catheter/ CVC(Central Venous Lines)
- An NG Tube (Nasogastric Tubes) is usually inserted into your loved ones stomach, in order to commence nutrition or to remove fluids
- Urine Output is usually measured hourly, after insertion of a Urinary Catheter
How long will your loved one remain in ICU?
Your loved one may need to remain in ICU for weeks to many months, depending on the severity of GBS.
If your loved one is to stay in Intensive Care for many months, due to ventilator dependency and is medically stable, also check out this site for more information www.intensivecareathome.com.au as home care with a much better Quality of Life for your loved one and for the Family could be an option.
Internet Links
- http://www.ninds.nih.gov/disorders/gbs/gbs.htm – National Institute of Neurological Disorders and Stroke(USA)
- http://www.nhs.uk/conditions/Guillain-Barre-syndrome/Pages/Introduction.aspx – National Health Service(NHS) in the UK
- Guillain-Barré Association on New South Wales
Any Questions?
Of course, if you have any questions or concerns, please discuss them with the ICU nurses and doctors.
All Intensive Care interventions and procedures carry a degree of potential risk even when performed by skilled and experienced staff. Please discuss these issues with the medical and nursing staff who are caring for your loved one.
The information contained on this page is general in nature and therefore cannot reflect individual Patient variation. It is meant as a back up to specific information which will be discussed with you by the Doctors and Nurses caring for your loved one. INTENSIVE CARE HOTLINE attests to the accuracy of the information contained here BUT takes no responsibility for how it may apply to an individual Patient. Please refer to the full disclaimer.
How can you have PEACE OF MIND, control, power and influence whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below! In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care! Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below!
In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care!
In your FREE reports you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 “killer” tips& strategies helping you to get on the right path to PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘BEHIND THE SCENES’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care(it’s not what you think)
Make sure you also check out our “blog” section for tips& strategies and also check out our “your questions answered” section where we answer your questions or send me an email to [email protected] with your questions!
Sincerely, your Friend
Patrik Hutzel
Related Articles:
- How much longer does my son need to stay in Intensive Care with Guillain-Barré Syndrome?
- How long can a breathing tube or an endotracheal tube can stay in?
- How long should a Patient be on a ventilator before having a Tracheostomy?
- How long is a Patient kept on a BIPAP machine in Intensive Care?
- What is an induced coma and why is my critically ill loved one in an induced coma?
- The 3 most dangerous mistakes that you are making but you are unaware of, if your loved one is a critically ill Patient in Intensive Care
- How to always achieve your goals whilst your loved one is critically ill in Intensive Care
- Why you must make up your own mind about your critically ill loved one’s situation in Intensive Care even if you’re not a doctor or a nurse!
- Follow this proven 5 step process on how to be in control and influential if your loved one is a long-term Patient in Intensive Care
- How to quickly take control and have real power and influence if your loved one is critically ill in Intensive Care
- Why does my loved one need a Tracheostomy in Intensive Care?
- Tracheostomy and weaning off the ventilator in Intensive Care, how long can it take?
- My sister has been in ICU for 21 weeks with Tracheostomy and still ventilated. What do we need to do?
- Severe lung failure and my aunty is not expected to survive…
- Be more selfish if your loved one is critically ill in Intensive Care
- 3 quick steps on how to position and prepare yourself well mentally, whilst your loved one is critically ill in Intensive Care
- How to get what you want whilst your loved one is critically ill in Intensive Care
- How to stay positive if your loved one is critically ill in Intensive Care
- 5 steps to become a better negotiator if your loved one is critically ill in Intensive Care
- 5 Ways to have control, power and influence while your loved one is critically ill in Intensive Care
- How to make sure that your values and beliefs are known whilst your loved one is critically ill in Intensive Care
- How to make sure that “what you see is always what you get” whilst your loved one is critically ill in Intensive Care
- What the doctors and the nurses behaviour in Intensive Care is telling you about the culture in a unit
- How long does it take to wake up from a Traumatic brain injury or severe head injury
- How to take control if your loved one has a severe brain injury and is critically ill in Intensive Care
- Family Meetings in Intensive Care or the Elephant in the Room
- What you need to do if your loved one is dying in Intensive Care(part one)
- What you need to do if your loved one is dying in Intensive Care(part two)
- Intensive Care at its best?
- How INTENSIVECAREHOTLINE.COM Can Help You
- What you and your Family need to do if your critically ill loved one is very sick in Intensive Care and faces an uncertain future
- How long can somebody stay in Intensive Care?
- My Family can’t agree on what’s best for my sister in Intensive Care…Help!
- My husband is dying in Intensive Care, but we need more time…
- My mother sustained serious brain damage after a stroke and she now is in multi- organ failure


