What is a central venous line or Central Venous Catheter?
In medicine, a central venous line(“central venous catheter”, “CVC”, “central line” or “central venous access catheter”) is a catheter with multiple openings(lumens) a the end tip, placed into a large vein in the neck (internal jugular vein), chest (subclavian vein or axillary vein) or groin (femoral vein). It is used to administer medication or fluids, obtain blood tests (Blood& Pathology tests in Intensive Care), and directly obtain cardiovascular measurements such as the central venous pressure(also known as ‘filling’ pressure.
The line that is inserted at the elbow is called a PICC (Peripherally Inserted Central Catheter), and the lines that enter the shoulder, neck or groin are called Central Venous Lines. The term central line will be used from this point on.
When the line is not in use, the access lines are ‘capped’ with a plastic bung and a clamp, in order to avoid blood leaking out of the line and in order to avoid infections. The central line is usually sutured(stitches) in at the entry point to the blood vessels and is also secured with a transparent dressing to keep the line clean and visible. The Central Venous line can be kept in for up to 10 days, but this can vary from ICU to ICU, as different protocols in different units apply. But the longer the Central venous line is kept in place, the higher the risk for an infection, caused by Bacteria moving into the blood stream. The infection risk can be diminished by changing the central line regularly.
Why does your loved one need a central line?
How is it inserted?
What are the risks of central lines?
Keeping the line clean
Publication Information
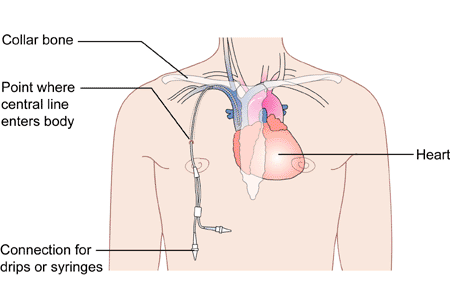

Why does your loved one need a central line ?
Indications for the use of central lines include:
- Monitoring of the central venous pressure (CVP) in acutely ill patients to quantify fluid balance
- Long-term Intravenous antibiotics
- Long-term Parenteral nutrition(TPN) especially in chronically ill patients
- Long-term pain medications
- Chemotherapy
- Drugs that are prone to cause phlebitis(inflammation of the veins) in peripheral veins, such as:
- Calcium chloride
- Chemotherapy
- Hypertonic saline
- Potassium chloride
- Amiodarone
- vasopressors, inotropes or vasodilators (e.g. epinephrine, Noradrenaline dopamine)
- Plasmapheres(removal, treatment, and return of components of blood plasma from blood circulation)
- Peripheral blood stem cell collections
- Haemodialysis or Haemofiltration(Dialysis Catheter, Dialysis Machines)
- Frequent blood draws
- Frequent or persistent requirement for intravenous access
- Need for intravenous therapy when peripheral venous access is impossible
- Blood and blood product transfusions
- Medication
- Rehydration
Central venous catheters usually remain in place for a longer period of time than other venous access devices, especially when the reason for their use is longstanding (such as total parenteral nutrition/TPN in a chronically ill Patient). For such indications, a Hickman line, a PICC line or a portacath may be considered because of their smaller infection risk. Sterile technique is highly important here, as a line may serve as a place of entry for pathogenic organisms, and the line itself may become infected with organisms such as Staphylococcus aureus.
How is it inserted?
The doctor or a nurse specialist performs the procedure, cleans the skin and applies local anesthetic if required. The location of the vein is then identified by landmarks or with the use of a small ultrasound device. A hollow needle is advanced through the skin until blood is aspirated; the color of the blood and the rate of its flow help distinguish it from arterial blood, suggesting that an artery has been accidentally punctured if the colour is light red and blood is ‘pumping out’. Ultrasound probably now represents the gold standard for central venous access and skills. Prior tothe procedure, your loved one my be given sedation so that your loved one is drowsy and relaxed during the procedure.
The line is then inserted using the Seldinger technique: a blunt guidewire is passed through the needle, then the needle is removed. A dilating device may be passed over the guidewire to slightly enlarge the tract. Finally, the central line itself is then passed over the guidewire, which is then removed. All the lumens of the line are aspirated (to ensure that they are all positioned inside the vein) and flushed. A Chest X-ray is typically performed afterwards to confirm that the line is positioned inside the superior vena cava and, in the case of insertion through the subclavian vein, that no pneumothorax was caused as a side effect.
A PICC line is also inserted in a sterile fashion.
- A tourniquet is applied to the arm and the area is cleaned and draped;
- Local anaesthetic is injected into the skin near the vein;
- A cannula is then inserted into the vein, the needle is removed, and the tourniquet is released;
- A wire is inserted through the cannula and further into the vein;
- A larger catheter is then inserted over the wire to enlarge the skin opening, and to hold the vein open;
- The wire is removed and all that remains in the arm is the catheter;
- The PICC is then thread up the arm vein through the catheter to a previously measured level; and
- The PICC is then secured with a Stat lock or dressing.
The injection of local anaesthetic is usually the part of the procedure that causes the most discomfort. Once the needle or cannula is sitting in the vein the remainder of the procedure is not painful. Some minor bleeding may be seen at the insertion site on the first day.
What are the risks of central lines?
As with most procedures there is a small risk of complications.
- Pneumothorax (accidental puncture of the lung) for central lines placed in the chest. The incidence is thought to be higher with subclavian vein catheterization. In catheterization of the internal jugular vein, the risk of pneumothorax can be minimized by the use of ultrasound guidance.
- Infection- is possible with any line, central or otherwise, and the risk increases with the age of the line. About one line in 20 will become infected. The signs of infection include redness, swelling and tenderness around the line as it enters the skin and fever or chills. If a line infection has occurred, usually the line has to be removed.
- venous thrombosis(blood clot in the veins)
Keeping the line clean
Prevention of infection is an important consideration. For this reason touching to central line is discouraged and anyone who does must wash their hands first. Cleanliness of the skin around the central line is paramount and it is not be touched unless hands have been washed prio to touching the line. The CVC dressing needs to be changed every 2-3 days or as needed.
Any Questions?
Of course, if you have any questions or concerns, please discuss them with the ICU nurses and doctors.
All Intensive Care interventions and procedures carry a degree of potential risk even when performed by skilled and experienced staff. Please discuss these issues with the medical and nursing staff who are caring for your loved one.
The information contained on this page is general in nature and therefore cannot reflect individual patient variation. It is meant as a back up to specific information which will be discussed with you by the Doctors and Nurses caring for your loved one. INTENSIVE CARE HOTLINE attests to the accuracy of the information contained here BUT takes no responsibility for how it may apply to an individual Patient. Please refer to the full disclaimer.
How can you have PEACE OF MIND, control, power and influence whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below! In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care! Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below!
In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care!
In your FREE reports you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 “killer” tips& strategies helping you to get on the right path to PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘BEHIND THE SCENES’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care(it’s not what you think)
Make sure you also check out our “blog” section for tips& strategies and also check out our “your questions answered” section where we answer your questions or send me an email to [email protected] with your questions!
Sincerely, your Friend
Patrik Hutzel
Related articles:


